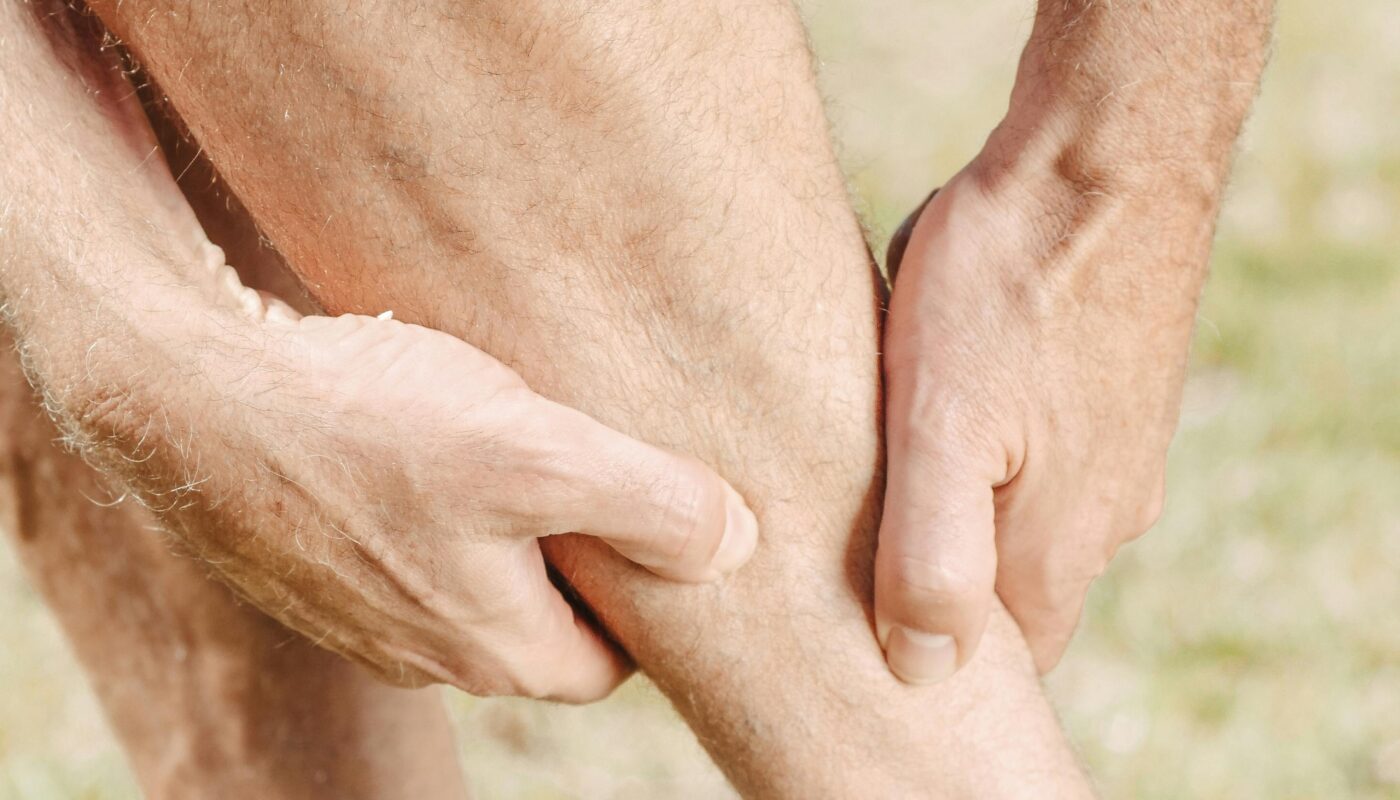
Rest is supposed to be restorative. It is what we instinctively turn to when something hurts. We sit down after a long day, lie back after exercise, or go to sleep hoping the discomfort will ease. Yet for many people, the opposite happens. They wake up stiff and aching. Their back throbs after a long drive. Their knees protest when they stand after sitting through a meeting. Instead of relief, rest seems to invite pain.
If you have ever wondered why pain can appear after resting, you are not alone. This experience is common across age groups and health conditions. It affects office workers, athletes, people with arthritis, individuals recovering from injury, and even those who consider themselves generally healthy. The discomfort may feel like stiffness, dull aching, tight pulling, burning, or even sharp jolts when movement resumes.
The important thing to understand is that pain after rest is not imaginary, and it is not a personal failure. It is often a predictable response rooted in physiology, biomechanics, and the way the nervous system processes signals. When you understand what is happening inside your body during periods of inactivity, the mystery begins to dissolve.
Rest Changes Circulation in Subtle but Powerful Ways
Movement keeps blood flowing efficiently. Every time your muscles contract, they help push blood back toward the heart. This “muscle pump” supports circulation and ensures tissues receive oxygen and nutrients while metabolic waste products are cleared away.
When you rest, especially in one position for an extended period, that pump slows down. Blood flow becomes more passive. In healthy individuals this change is usually mild, but in those with underlying circulation issues, inflammation, or muscle tightness, reduced flow can allow metabolic byproducts to accumulate. These substances can irritate surrounding tissues and nerve endings.
This is one reason why someone might feel relatively comfortable while walking but experience throbbing or aching once they sit down. The moment movement stops, the supportive effects of circulation diminish. In areas already prone to strain, such as the lower back or neck, this shift can be enough to trigger discomfort.
Stiffness Builds Quietly During Inactivity
Muscles and connective tissues are dynamic. They are designed to lengthen and shorten, to glide and adapt. When held in a static position, they begin to adjust to that position. Over time, tissues can shorten slightly or become less pliable. This process is subtle but cumulative.
Imagine sitting at a desk for hours with your hips flexed and shoulders rounded forward. Those muscles begin to adapt to that shortened posture. When you stand up, they resist sudden lengthening. The resistance may register as stiffness or even sharp pain.
Similarly, during sleep, if the neck is unsupported or the spine is not aligned properly, certain muscles remain under low-level strain. By morning, they may feel tight and tender. The pain is not necessarily a sign of damage. Often it is the body reacting to prolonged stillness combined with imperfect positioning.
Inflammation Can Intensify During Rest
It seems logical that rest would reduce inflammation. In many acute injuries, that is true. However, in chronic inflammatory conditions, rest can sometimes allow inflammatory processes to become more noticeable.
People with osteoarthritis frequently report morning stiffness. Overnight, joints remain relatively immobile. Synovial fluid, which lubricates joints, does not circulate as effectively without movement. Inflammatory chemicals may accumulate within joint spaces. Upon waking, the first steps can feel stiff and painful.
This pattern is widely recognized in clinical research and patient education materials from organizations such as Mayo Clinic and National Institutes of Health, both of which note that inflammatory joint conditions often produce worse symptoms after periods of inactivity.
The key insight here is that gentle movement, not prolonged rest, often improves symptoms in these cases. Motion helps distribute joint fluid and reduce inflammatory buildup.
The Nervous System Does Not “Switch Off” During Rest
Pain is not produced only in muscles and joints. It is processed and interpreted by the nervous system. When pain becomes chronic, the nervous system can become sensitized. This means it reacts more strongly to stimuli that might otherwise feel neutral.
During activity, the brain receives multiple sensory inputs: movement, balance, visual cues, and environmental interaction. These signals can partially “compete” with pain signals. When you stop moving and lie quietly, there are fewer competing inputs. The brain may become more aware of discomfort that was already present but less noticeable.
In conditions like fibromyalgia or chronic back pain, central sensitization plays a significant role. The nervous system becomes hyper-alert. Resting in silence may make pain feel louder, not because tissues are worsening, but because attention and neural amplification increase.
This phenomenon can be deeply frustrating. It may lead people to fear rest or believe something serious is happening. Understanding that the nervous system contributes to this experience can reduce anxiety and open the door to strategies that calm neural overactivity.
Delayed Onset Muscle Soreness Peaks After Rest
After unfamiliar or intense exercise, muscle fibers develop microscopic tears. This is a normal part of adaptation and strengthening. The repair process triggers inflammation and sensitivity known as delayed onset muscle soreness, often peaking 24 to 72 hours after activity.
What is interesting is that the pain is often most noticeable after rest. Sitting for a while and then standing up may produce sharp stiffness in the thighs. Rolling out of bed can feel surprisingly uncomfortable after leg day at the gym.
The soreness did not originate during rest, but rest makes it more apparent. Muscles that have been idle temporarily lose warmth and flexibility. The first movements stretch healing fibers, producing discomfort.
In this situation, the pain signals recovery rather than harm. Gentle activity, hydration, and adequate sleep usually ease the symptoms within a few days.
Spinal Discs and Pressure Redistribution
The spine undergoes subtle changes during rest, particularly during sleep. When lying down, pressure on spinal discs shifts. Discs rehydrate overnight, slightly increasing in volume. For individuals with disc degeneration or minor bulges, this rehydration can temporarily increase internal pressure.
Upon waking, bending forward or twisting may provoke discomfort. As the day progresses and gravity compresses the discs again, the pain may lessen.
This pattern is common in people with chronic low back pain. It does not automatically indicate serious pathology. However, persistent morning pain accompanied by neurological symptoms such as numbness or weakness should be evaluated by a healthcare professional.
Joint Fluid Dynamics and the “Startup Pain” Effect
Many individuals with knee or hip arthritis describe “startup pain.” They feel relatively comfortable once walking, but the first few steps after sitting are painful.
Inside joints, synovial fluid provides lubrication. During movement, this fluid circulates efficiently. During inactivity, it becomes less evenly distributed. Cartilage surfaces may experience slightly increased friction when movement resumes. The initial steps can feel stiff and sharp until lubrication improves.
Understanding this effect helps explain why gentle stretching or slow pacing after rest often reduces discomfort within minutes.
The Psychological Component of Rest
Rest often occurs in quiet moments: at night, during breaks, or when alone. In these settings, attention turns inward. Without distraction, the brain may focus more intently on bodily sensations.
Anxiety can amplify pain perception. If someone expects pain after rest, the anticipation itself can heighten neural sensitivity. Sleep disturbances also influence pain thresholds. Poor-quality sleep is strongly associated with increased next-day pain levels.
Research frequently cited by institutions like the Harvard Health Publishing highlights the bidirectional relationship between sleep and pain. Insufficient or fragmented sleep lowers pain tolerance, making normal stiffness feel more intense.
In this way, rest and pain can form a cycle. Pain disrupts sleep. Poor sleep increases pain. Breaking that cycle often requires addressing both physical and psychological factors.
Postural Collapse and Loss of Muscular Support
While standing or walking, certain muscles actively stabilize joints. During prolonged rest, especially in slouched positions, supportive muscles disengage. The spine may settle into less optimal alignment.
For someone with weak core musculature, lying on a soft mattress or sitting in a sagging chair may place additional strain on ligaments and passive structures. Over time, these tissues become irritated. When the person moves again, pain appears.
Strengthening supportive muscles and improving ergonomic alignment can dramatically reduce this type of post-rest discomfort.
Circulation and Nerve Compression During Sleep
Sleeping positions sometimes compress nerves. For example, lying with the wrist bent can irritate the median nerve. Sleeping on one shoulder for hours may compress soft tissues and cause morning numbness or tingling.
In most cases, these symptoms resolve quickly after repositioning and moving around. However, repeated nerve compression can lead to more persistent irritation.
Choosing supportive pillows and avoiding extreme joint angles during sleep can reduce these issues.
Chronic Conditions That Commonly Produce Pain After Rest
Several medical conditions are particularly associated with rest-related pain. Osteoarthritis produces stiffness after inactivity. Rheumatoid arthritis often causes prolonged morning stiffness due to autoimmune inflammation. Ankylosing spondylitis, an inflammatory spinal condition, characteristically worsens with rest and improves with movement.
Tendinopathies, such as Achilles tendon pain, frequently hurt most during the first steps in the morning. The tendon stiffens overnight and gradually loosens with activity.
Recognizing patterns can help distinguish between benign stiffness and symptoms that require medical evaluation.
When Pain After Rest Signals Something More Serious
Although pain after resting is often harmless, certain warning signs should not be ignored. Persistent severe pain, progressive weakness, unexplained weight loss, fever, or loss of bowel or bladder control require immediate medical assessment. Sudden onset of intense pain after trauma also warrants urgent evaluation.
Most cases, however, fall into a manageable category where lifestyle modifications and targeted therapy provide relief.
Practical Strategies to Reduce Pain After Rest
The solution to post-rest pain is rarely complete inactivity. Instead, gentle, intentional movement tends to be more effective.
Starting the day with slow stretches rather than abrupt movements allows tissues to warm gradually. Light walking increases circulation and distributes joint fluid. Core strengthening improves spinal support. Regular breaks from sitting prevent stiffness from accumulating.
Sleep environment adjustments can also make a difference. A supportive mattress, properly sized pillow, and neutral spinal alignment reduce strain during the night.
Hydration plays a subtle but meaningful role. Dehydrated tissues may feel tighter and more irritable. Balanced nutrition supports muscle recovery and reduces systemic inflammation.
Stress reduction techniques, including breathing exercises and mindfulness, calm the nervous system. When neural sensitivity decreases, pain intensity often follows.
Why Movement Is Often the Best Medicine
The paradox of pain after rest reveals an important truth: the human body is designed for movement. Joints depend on motion for lubrication. Muscles rely on contraction for circulation. The nervous system benefits from varied sensory input.
Rest remains essential for healing and recovery. The key is balance. Prolonged immobility can be as problematic as overexertion.
By shifting from a mindset of “rest completely until pain disappears” to one of “rest wisely and move gently,” many people find their symptoms become more manageable.
Understanding Replaces Fear
One of the most distressing aspects of pain after rest is uncertainty. People may worry that the pain indicates worsening damage. They may become hesitant to move, creating further stiffness and discomfort.
Education changes that narrative. Knowing that stiffness after sleep often reflects inflammation dynamics or muscle adaptation reduces anxiety. Recognizing that the nervous system amplifies sensations during stillness empowers individuals to respond calmly.
When fear decreases, muscle tension often decreases as well. This alone can reduce pain intensity.
A Balanced Approach to Rest and Recovery
Pain appearing after rest does not mean rest is harmful. It means rest interacts with your body’s physiology in complex ways. Circulation slows, inflammation shifts, tissues stiffen, and the nervous system becomes more attentive.
In many cases, the remedy is not more rest, but better movement patterns, improved posture, supportive sleep habits, and nervous system regulation.
If pain persists or worsens despite these strategies, professional evaluation ensures that underlying conditions are addressed appropriately. But for many people, simple adjustments restore comfort and confidence.
Pain after resting is a common experience. It reflects how dynamic and responsive the body truly is. When understood, it becomes less alarming and more manageable. By embracing balanced activity, mindful rest, and supportive habits, you can reduce the likelihood that stillness will trigger discomfort and instead allow rest to serve its intended purpose: recovery and renewal.
Sources: Mayo Clinic article on arthritis morning stiffness; National Institutes of Health overview on chronic pain mechanisms; Harvard Health Publishing article on sleep and pain relationship; Cleveland Clinic article on delayed onset muscle soreness.