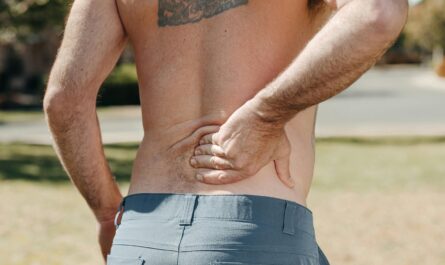
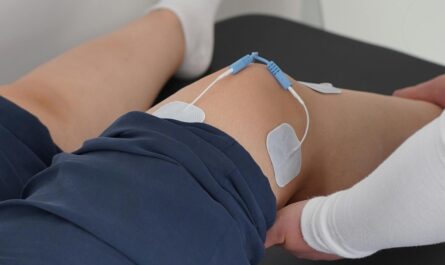
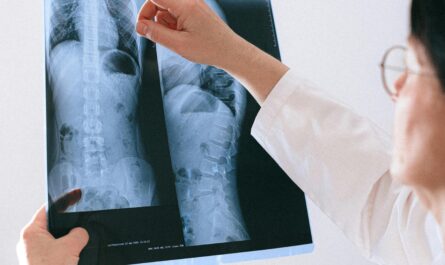
Pain is usually expected to be temporary. When the body is injured, pain appears as a warning signal, guiding a person to rest, protect the injured area, and allow healing to take place. In most situations, once the tissues recover, the pain fades and the body return to normal. However, for many people, pain does not disappear when it should. Instead, it stays for months or even years, gradually becoming part of daily life. When pain lasts this long, it does not remain the same as it was in the beginning. Long-standing pain slowly changes the way the body reacts, the way the nervous system sends signals, and the way the brain interprets sensations. Over time, the body adapts to pain in ways that can make the experience more intense, more sensitive, and more difficult to control.
Long-lasting pain, often called chronic pain, is not simply prolonged discomfort. It becomes a condition that affects the entire system. The nervous system, muscles, immune responses, hormones, and even emotional reactions begin to shift. These changes happen gradually, often without being noticed at first, but they can eventually make the body respond differently to touch, movement, stress, and even normal daily activities. Understanding how long-standing pain changes the body helps explain why some pain becomes persistent and why recovery can take longer than expected.
Pain exists as part of the body’s protection system. Special nerve endings detect damage or potential harm and send signals through the spinal cord to the brain. The brain then creates the feeling of pain so the person reacts quickly. This system is designed to keep the body safe, not to keep it suffering. When healing is complete, the signals are supposed to stop. But when pain continues for a long time, the nervous system stays active longer than it should, and this constant activity can slowly change the way the system works.
When pain signals travel repeatedly through the same nerve pathways, the body begins to adapt to those signals. The brain and spinal cord become more efficient at sending and receiving them. This ability of the nervous system to change is called neuroplasticity. Neuroplasticity helps people learn new skills and recover from injury, but it can also make the body learn pain. The more often pain signals are used, the stronger those pathways can become. Over time, the body may react faster and more strongly to the same stimulus, even if the original injury has already healed.
As this process continues, the nervous system can become more sensitive. Sensitivity in this case does not mean emotional sensitivity, but physical sensitivity in the way nerves respond to stimulation. A person who once felt mild discomfort may start to feel stronger pain from the same movement or touch. In some cases, sensations that normally would not hurt at all can begin to feel painful. This change happens because the nervous system starts to amplify signals instead of filtering them. The body’s internal “volume control” for pain becomes turned up higher than normal, and it does not easily return to its original level.
Over time, the brain itself begins to change. The brain is constantly adapting to what it experiences, and when pain is present for long periods, the brain reorganizes the way it processes signals. Areas involved in pain detection may become more active, while areas that help reduce pain may become less effective. This process is sometimes called central sensitization, meaning the central nervous system becomes more reactive. When this happens, pain may continue even when there is no clear injury because the system that produces pain has become easier to activate.
In long-standing pain, the brain can also become more alert to danger signals. When pain happens repeatedly, the brain learns to expect it. This expectation makes the nervous system more prepared to react, even when there is no real threat. The body may stay in a protective state, muscles may remain tense, and the mind may become more focused on discomfort. This is not something a person chooses. It is the result of the brain trying to protect the body, but the protection system becomes too active and begins to react to normal sensations as if they are harmful.
The changes caused by long-standing pain are not limited to the brain and nerves. Muscles and joints also begin to react differently. When pain lasts for a long time, people naturally change the way they move. They may avoid certain positions, limit activity, or hold their body in ways that reduce discomfort. These protective movements are helpful in the short term, but over time they can lead to stiffness, weakness, and reduced flexibility. Muscles that are not used regularly can become tight or sensitive, and joints may lose their normal range of motion. As a result, the body can become more vulnerable to pain even during simple activities.
Long-lasting pain can also affect the immune system. When the body is injured, the immune system releases chemicals that cause inflammation, helping the healing process. In normal situations, this inflammation decreases once recovery is complete. However, when pain becomes chronic, the immune system may stay active longer than necessary. Certain immune cells in the nervous system can continue releasing substances that make nerve endings more sensitive. This ongoing activity can keep pain signals active even when there is no longer any damage to repair. Because the nervous system and immune system are closely connected, this prolonged sensitivity can spread and affect different parts of the body.
Another important change occurs in the body’s stress response. Pain that continues for months or years keeps the body in a state of alertness. Stress hormones may be released more often, and the nervous system may remain in a defensive mode. This can affect sleep, energy levels, digestion, and mood. Many people with long-standing pain feel tired even after resting, or tense even when nothing stressful is happening. The body becomes used to being on guard, and it may react strongly to situations that would not have caused discomfort before.
Hormonal balance can also be affected. When the body stays in a constant stress state, the systems that control hormones may not work as smoothly as they should. This can influence appetite, temperature regulation, fatigue, and emotional stability. These changes do not mean the pain is only in the mind. They show that long-standing pain affects the entire body, not just the place where the pain is felt.
Emotional and mental reactions also play a role in how the body changes over time. Living with pain for a long period can lead to frustration, worry, or sadness. These feelings are natural, but they can also influence how the brain processes pain signals. When the mind expects pain or feels stressed, the nervous system can become more sensitive. This makes the pain feel stronger and more constant. The connection between mind and body means that physical and emotional reactions influence each other, especially when pain lasts a long time.
One of the most difficult aspects of long-standing pain is that the changes happen slowly. A person may not notice at first that their body is reacting differently. The pain may start in one place, then become more sensitive, then begin to affect sleep, mood, and movement. Over time, the body adapts to the presence of pain. The nervous system becomes better at producing pain signals, muscles become more protective, the brain becomes more alert, and the stress system stays active longer. These adaptations are the body’s way of responding to repeated signals, but they can make the pain feel more persistent.
Understanding this process helps explain why long-term pain can continue even after medical tests show no clear injury. The original problem may have healed, but the nervous system has changed. The body has learned the pattern of pain, and it may continue reacting in the same way. This does not mean the pain is imagined. It means the system that produces pain has become more sensitive through repeated use.
The important thing to remember is that the body’s ability to change works in both directions. Just as the nervous system can learn pain, it can also learn to reduce it. Because the brain and nerves are adaptable, the body can slowly move back toward balance when the right conditions are created. This process may take time, and it often requires patience, but the changes caused by long-standing pain are not always permanent.
When people understand that chronic pain can reshape the body’s reactions, they often feel less confused about why their symptoms behave the way they do. Long-standing pain is not simply pain that stayed too long. It is pain that gradually taught the body to react differently. The nervous system learned to stay alert, the muscles learned to stay tense, and the brain learned to expect danger. With time and the right approach, the body can also learn new patterns, but the first step is understanding how deeply long-term pain can influence the way the body works.
Long-standing pain changes the body slowly, quietly, and often without warning. What begins as a simple injury can become a complex reaction involving the brain, nerves, muscles, immune system, and emotions. The longer pain continues, the more the body adapts to it, and the more different the reactions can become. Recognizing these changes does not remove the pain, but it helps explain why the experience feels different than it did at the beginning, and why healing sometimes requires more than treating the original injury.
Sources:
Mayo Clinic Press – What is central sensitization and how does it relate to pain? | MSD Manual – Chronic Pain | Cleveland Clinic Journal of Medicine – Central sensitization, chronic pain, and other symptoms | PubMed – Neuroinflammation and chronic pain mechanisms | Cleveland Clinic – Central Pain Syndrome