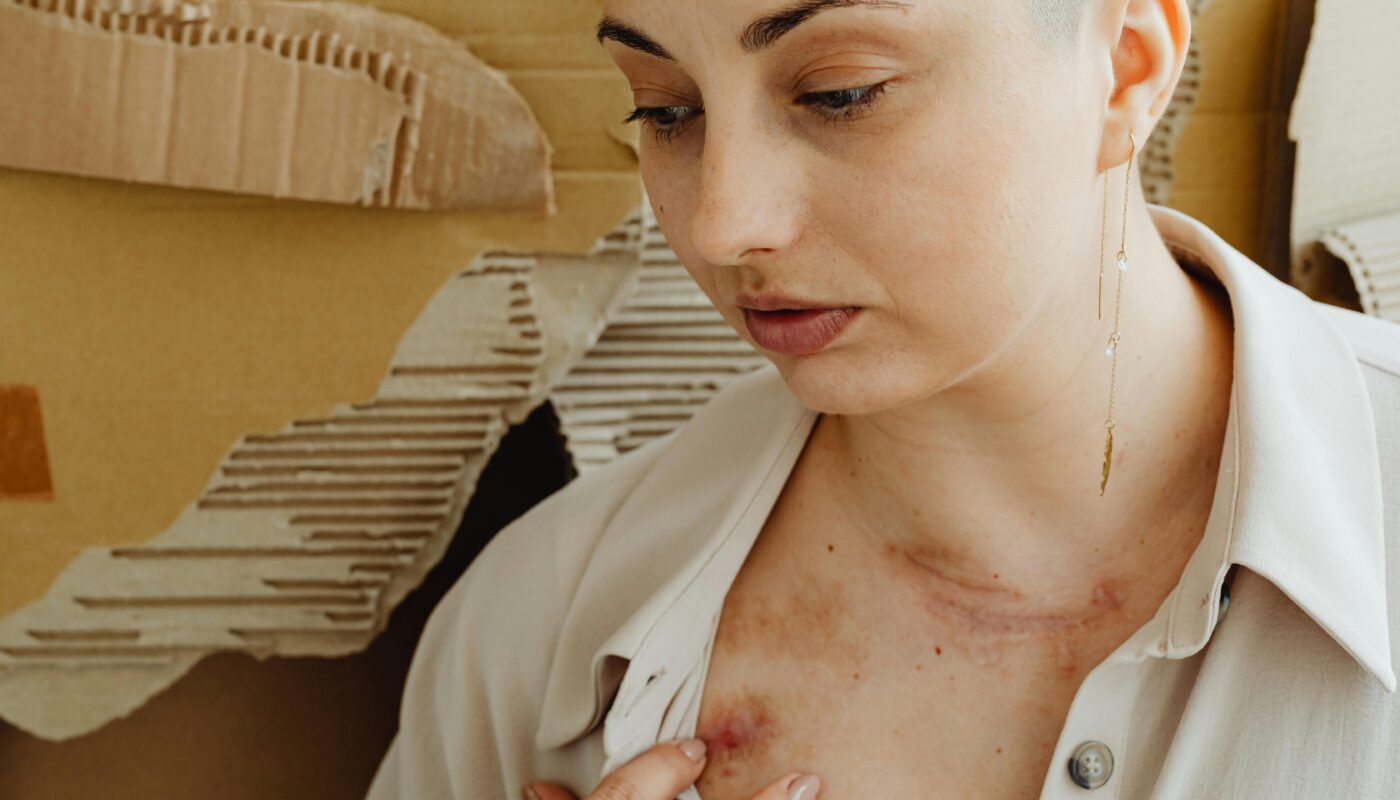
Healing is often imagined as a clean finish line. The cast comes off. The stitches dissolve. The infection clears. The scan shows no abnormality. The doctor says, “You’re healed.” Yet for many people, this moment does not bring the relief they expected. Instead, it introduces a confusing and deeply frustrating reality: the body may be medically healed, but pain lingers.
Post-recovery pain is one of the most misunderstood experiences in medicine. It challenges the simple belief that once tissue repairs itself, comfort automatically returns. For countless individuals recovering from surgery, injury, childbirth, illness, or even a severe inflammatory episode, discomfort persists beyond the expected healing window. This can create anxiety, self-doubt, and fear that something has gone wrong. In some cases, patients are told that “everything looks fine,” which only deepens their distress when pain continues.
The truth is more complex and more human. Healing does not always mean comfort because pain is not solely a signal of damage. It is a protective output of the nervous system shaped by biology, psychology, memory, and environment. When we understand this, post-recovery pain becomes less mysterious and more manageable.
To understand why pain can remain after healing, we must first separate two processes that are often confused: tissue repair and nervous system recalibration. Tissue healing follows relatively predictable stages. Inflammation appears first, recruiting immune cells to clean damaged areas. New tissue forms. Remodeling strengthens the repair. Depending on the injury, this may take weeks or months. However, the nervous system does not always follow the same timeline. During injury, pain signals repeatedly travel from the affected area to the spinal cord and brain. These repeated signals can increase the sensitivity of pain pathways. In effect, the system becomes highly efficient at detecting threat.
This process, often referred to as sensitization, can persist even after tissues recover. Nerves that were once triggered only by strong stimuli may now respond to mild pressure, temperature changes, or normal movement. The brain, which has learned to associate certain motions or sensations with danger, may continue generating pain as a protective measure. In this way, the body is not malfunctioning; it is being overly cautious.
Inflammation also plays a role in lingering discomfort. While acute inflammation is essential for healing, inflammatory chemicals can sometimes remain elevated longer than expected. These substances can irritate nearby nerve endings, making them more reactive. Even subtle residual inflammation, invisible on standard imaging tests, can amplify sensitivity. For some individuals, especially those with autoimmune tendencies or metabolic stress, this inflammatory sensitivity can persist quietly in the background.
Nerve healing itself can contribute to post-recovery pain. When nerves are stretched, compressed, or cut during injury or surgery, they regenerate slowly. During regeneration, abnormal signaling can occur. People may experience tingling, burning, stabbing sensations, or hypersensitivity. These symptoms do not necessarily mean the original injury is still present. They may reflect the complex process of nerve repair. Unfortunately, nerve regeneration can take months, and in some cases, altered signaling becomes chronic.
Beyond the biological mechanisms, psychological and emotional factors strongly influence post-recovery pain. Pain is processed in the brain regions that also regulate fear, attention, and emotion. If an injury was traumatic or frightening, the memory of that event can remain active. When the brain anticipates pain, it becomes more vigilant. This hypervigilance increases sensitivity to bodily sensations. Normal sensations that would otherwise go unnoticed may be interpreted as threatening.
Anxiety can heighten pain perception by increasing muscle tension and activating stress hormones. When muscles tighten around a previously injured area, blood flow can decrease, creating genuine discomfort. Stress hormones can also amplify inflammatory responses. Depression may reduce pain tolerance, making sensations feel more intense. Catastrophic thinking, such as assuming that persistent discomfort means permanent damage, reinforces the pain cycle. The brain, seeking to protect the body, continues to generate pain signals as a warning.
Social factors also influence the experience of post-recovery pain. Supportive environments often help people regain confidence in movement and daily activities. Conversely, environments filled with doubt or pressure can increase stress. Cultural beliefs about pain shape expectations. In some communities, expressing pain is discouraged, leading individuals to internalize distress. In others, pain may be strongly medicalized, causing individuals to interpret every sensation as a sign of pathology. Both extremes can complicate recovery.
Movement patterns after injury are another overlooked contributor. During the painful phase of an injury, people naturally guard the affected area. They move differently, sometimes unconsciously. While protective in the short term, these altered patterns can create secondary strain in surrounding muscles and joints. Even after healing, these compensatory habits may persist, leading to stiffness or new discomfort. The original injury may be resolved, but the body’s movement habits still reflect it.
Surgical recovery provides a common example. A person who undergoes abdominal surgery may heal well structurally, yet months later still experience pulling or tightness around the scar. Scar tissue, while strong, is less flexible than original tissue. It can adhere to surrounding layers, restricting movement slightly. This mechanical restriction can produce sensations interpreted as pain. Gentle rehabilitation and mobility exercises often help, but without them, discomfort can persist despite successful healing.
Childbirth offers another illustration. After delivery, tissues gradually return to pre-pregnancy states. However, hormonal changes, pelvic floor stress, sleep deprivation, and emotional adjustments create a complex recovery environment. Some women report lingering pelvic or back pain long after medical clearance. In such cases, structural healing may have occurred, but muscle imbalances, nerve sensitivity, and hormonal fluctuations contribute to ongoing discomfort.
Post-infectious pain is another phenomenon gaining recognition. Some individuals recover from viral or bacterial illnesses only to experience widespread aches and fatigue afterward. While active infection is gone, the immune system may remain in a heightened state. The nervous system, having endured prolonged stress, may stay sensitized. This does not imply ongoing infection; rather, it reflects the body’s difficulty in returning fully to baseline.
One of the greatest challenges of post-recovery pain is validation. When diagnostic tests appear normal, patients may feel dismissed. They might begin questioning their own perceptions. This doubt increases stress, which in turn worsens pain. Breaking this cycle requires education. Understanding that pain is an output influenced by many systems can be empowering. It shifts the narrative from “Something is wrong with me” to “My nervous system needs support recalibrating.”
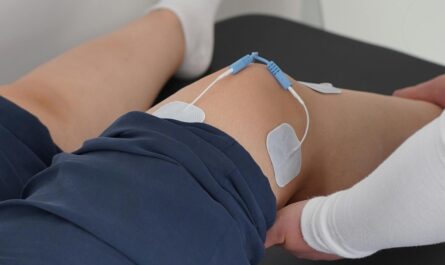
Management of post-recovery pain rarely depends on a single solution. Instead, it benefits from a comprehensive approach. Gradual reintroduction of movement is often central. Movement sends signals of safety to the brain. When performed progressively and without panic, it helps retrain pain pathways. Physical therapy tailored to the individual’s condition can restore strength, flexibility, and confidence.
Mind-body techniques also play a significant role. Practices such as mindful breathing, meditation, and gentle yoga help calm the stress response. When the nervous system shifts from a state of vigilance to one of safety, pain intensity often decreases. Sleep optimization is equally important. Sleep deprivation lowers pain thresholds and impairs tissue recovery. Establishing consistent sleep patterns supports overall healing.
Nutrition influences inflammation and nerve health. Diets rich in omega-3 fatty acids, antioxidants, and whole foods may help regulate inflammatory processes. Hydration supports tissue elasticity and cellular repair. While diet alone does not eliminate post-recovery pain, it contributes to an internal environment conducive to comfort.
Psychological therapies, especially cognitive behavioral therapy and acceptance-based approaches, have demonstrated effectiveness in reducing persistent pain. These therapies do not suggest that pain is imaginary. Rather, they help individuals change their relationship to pain, reducing fear and catastrophic thinking. When fear diminishes, the nervous system often follows.
Medication may be useful in certain cases, particularly when nerve pain is pronounced. However, relying solely on medication without addressing movement, stress, and psychological factors rarely provides lasting relief. Post-recovery pain is multidimensional, and treatment must reflect that complexity.
It is also essential to distinguish between benign post-recovery discomfort and warning signs that require further evaluation. Worsening pain, new neurological symptoms, fever, swelling, or functional decline should prompt medical reassessment. While persistent pain is common, it should not be automatically dismissed. Open communication between patient and provider ensures safety while preventing unnecessary alarm.
The future of pain science is increasingly focused on neuroplasticity, the brain’s ability to change and adapt. Just as the nervous system can learn pain, it can also unlearn it. Emerging therapies aim to harness this adaptability. Graded exposure to feared movements, sensory retraining, and even virtual reality interventions are being explored to recalibrate pain pathways. The message is hopeful: persistent pain does not have to be permanent.
Perhaps the most important shift needed is cultural. Society often equates resilience with silence and healing with perfection. In reality, recovery is rarely linear. There are setbacks, fluctuations, and periods of doubt. Recognizing that comfort may lag behind structural healing allows individuals to approach recovery with patience rather than panic.
For someone experiencing post-recovery pain, the emotional burden can be as heavy as the physical sensation. They may feel betrayed by their body or misunderstood by others. Acknowledging this emotional layer is crucial. Compassion, both from healthcare providers and from oneself, forms a cornerstone of healing.
Healing is not just the closing of a wound. It is the gradual restoration of trust between the body and the brain. When injury occurs, that trust is shaken. The nervous system becomes protective. After tissues mend, the system must relearn that safety has returned. This relearning takes time, guidance, and reassurance.
Understanding post-recovery pain reframes the experience from a sign of failure to a phase of adjustment. The body is not broken; it is recalibrating. The brain is not inventing pain; it is attempting to prevent harm. With appropriate support, most people can reduce persistent discomfort and regain full function.
The path to comfort after healing may be longer than expected, but it is navigable. Education reduces fear. Movement restores confidence. Emotional support builds resilience. Over time, the nervous system softens its protective stance, and comfort becomes more consistent.
Post-recovery pain reminds us that healing is not merely biological. It is neurological, psychological, and social. True recovery addresses all these layers. When we embrace this broader understanding, we move closer to a model of care that validates experience while guiding individuals toward lasting relief.
Healing does not always mean immediate comfort. But with knowledge, patience, and comprehensive care, comfort can follow.
Sources:
Harvard Health Publishing – Why acute pain sometimes becomes chronic pain; Mayo Clinic – Chronic pain: Diagnosis and treatment; National Institute of Neurological Disorders and Stroke – Pain: Hope Through Research; American Chronic Pain Association – Pain Basics and Pain Management Strategies