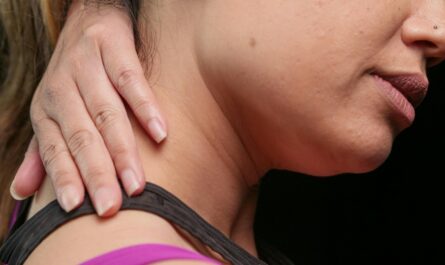
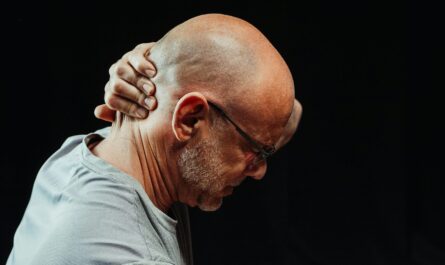
Pain is supposed to be simple. You injure your knee, your knee hurts. You burn your finger, your finger throbs. The location of pain usually tells you where the problem is. But sometimes the body breaks that rule. Sometimes your shoulder aches even though the problem is in your gallbladder. Sometimes your jaw tightens and throbs when the real issue is your heart. Sometimes your back screams in protest when the cause lies deep in your abdomen.
This phenomenon is called referred pain, and it is one of the most misunderstood experiences in medicine. It is not imaginary. It is not “in your head.” It is not random. It is a predictable neurological event rooted in how your nervous system is wired.
Understanding referred pain is more than medical curiosity. It can prevent misdiagnosis, reduce unnecessary anxiety, and in some cases, save lives. When pain appears in a place that seems unrelated to any injury, confusion follows. People treat the wrong area. They massage, stretch, ice, or ignore it. Meanwhile, the true source continues to signal distress. This article explores what referred pain truly is, why it happens, how it feels, and why recognizing it matters.
Referred pain is pain perceived in a location different from its actual source. The origin of the painful stimulus lies in one part of the body, but the brain interprets it as coming from another area. The sensation feels real and localized, yet it is neurologically misdirected.
This is not the same as radiating pain. Radiating pain spreads outward from its source along a continuous path, such as sciatic pain moving down the leg. Referred pain, by contrast, does not follow a clear pathway from origin to perception. It appears in a separate area altogether, sometimes distant from the true cause.
The classic example involves the heart. During a heart attack, pain may be felt in the left arm, shoulder, neck, jaw, or upper back instead of—or in addition to—the chest. Many people are unaware that jaw or arm discomfort can signal cardiac distress. That misunderstanding has cost lives. The heart is not located in the arm, yet the nervous system allows signals from the heart to be interpreted as arm pain.
To understand why this happens, we must look at how pain signals travel. Pain begins with specialized nerve endings called nociceptors. These receptors detect tissue damage, inflammation, or harmful stimuli. When activated, they send electrical signals along peripheral nerves to the spinal cord. From there, signals ascend through the spinal cord to the brain, where they are processed and interpreted.
Here is where complexity begins. The spinal cord is not a simple one-lane highway. It is more like a busy interchange. Nerve fibers from different tissues—skin, muscles, joints, and internal organs—often converge onto the same second-order neurons in the spinal cord. This means signals from multiple body regions share overlapping pathways.
One widely accepted explanation for referred pain is the convergence-projection theory, described in medical literature and educational references such as Cleveland Clinic and Encyclopædia Britannica. According to this theory, sensory fibers from an internal organ and sensory fibers from a region of skin may synapse onto the same spinal neuron. When the brain receives incoming signals from that shared neuron, it may misinterpret the source. Because the brain is more accustomed to receiving pain signals from the skin or musculoskeletal system than from internal organs, it often attributes the signal to the more familiar location.
In simpler terms, the brain makes its best guess. And sometimes that guess is wrong.
Internal organs add another layer of complexity. Visceral pain—pain from organs—is typically diffuse, vague, and poorly localized. Unlike skin, which has a high density of sensory receptors, organs have fewer pain receptors and provide less precise information. When visceral signals converge with somatic (body wall) signals in the spinal cord, the brain may default to the somatic region for localization.
Embryology also plays a role. During early development, certain organs and skin regions share common spinal segments. Even though organs migrate during growth, their nerve supply remains connected to the same spinal levels. As a result, pain from those organs may be referred to skin areas innervated by the same segments. This explains why gallbladder irritation can cause right shoulder pain or why early appendicitis may present as pain around the navel before shifting lower.
The phenomenon is so consistent that clinicians map referred pain patterns as diagnostic tools. Textbooks and educational platforms like Healthline describe common referral zones to help patients understand unusual pain presentations.
Referred pain does not always feel sharp or electric. Often it is dull, aching, deep, or pressure-like. It may feel difficult to pinpoint. Some describe it as a heavy discomfort rather than a stabbing sensation. It may wax and wane. It may not respond to local treatments such as massage or stretching because the painful tissue is not actually located where the sensation is perceived.
Take the gallbladder as an example. When inflamed, it can irritate the diaphragm. The diaphragm shares nerve pathways with the shoulder region through the phrenic nerve. The brain interprets diaphragmatic irritation as shoulder discomfort. A person may spend days treating their shoulder with heat and rest, unaware that gallstones are the true issue.
Kidney stones offer another example. Pain may begin in the flank and radiate toward the groin. Although this pattern can feel like a spreading sensation, much of it is referred pain resulting from shared nerve segments in the lower thoracic and upper lumbar spinal cord.
Dental infections can cause headaches. Sinus inflammation can produce tooth pain. Pancreatic inflammation can manifest as back pain. The patterns may seem mysterious, but they follow neurological logic.
One reason referred pain causes anxiety is its unpredictability. When pain appears in an unexpected location, the mind searches for explanation. Without understanding referred pain, people often assume muscle strain or minor injury. They may ignore warning signs. Conversely, unexplained pain may trigger catastrophic thinking. Knowledge reduces both extremes.
It is important to distinguish referred pain from neuropathic pain. Neuropathic pain arises from damage to nerves themselves, often producing burning, tingling, or electric sensations. Referred pain, by contrast, results from intact nerves transmitting signals that are misinterpreted centrally. The wiring is functioning, but the interpretation is flawed.
Chronic pain conditions complicate the picture further. Repeated stimulation can lead to central sensitization, a state in which spinal neurons become hyperresponsive. When this occurs, pain may spread beyond its original boundaries. Although central sensitization differs from classic referred pain, overlapping mechanisms exist. The nervous system becomes more efficient at amplifying signals, and perception widens.
Understanding referred pain also requires acknowledging that pain is ultimately constructed by the brain. The brain integrates incoming sensory data with prior experience, context, and expectations. It produces a perception that is meant to protect you. Sometimes that protective system errs on the side of caution.
This interpretive process is evident in phenomena like phantom limb pain, where individuals feel pain in an amputated limb. Although not identical to referred pain, both illustrate that pain location is a product of neural representation rather than a simple physical map.
Clinically, referred pain presents diagnostic challenges. A patient with shoulder discomfort might receive physical therapy for weeks before imaging reveals gallbladder disease. A patient with jaw tightness may visit a dentist when cardiac evaluation is urgently needed. Physicians are trained to look beyond location and assess accompanying symptoms, risk factors, and pattern consistency.
Timing, associated symptoms, and triggers matter. Cardiac referred pain often appears with shortness of breath, sweating, nausea, or chest pressure. Gallbladder pain frequently follows fatty meals. Kidney stone pain is typically severe and colicky. Patterns tell a story.
Referred pain can also occur in musculoskeletal contexts. Trigger points in muscles may cause discomfort in distant areas. For example, tight neck muscles can produce pain behind the eye or at the temple. In these cases, the referral mechanism is more localized within musculoskeletal nerve pathways rather than visceral-somatic convergence.
The emotional impact of referred pain should not be overlooked. When pain feels disconnected from any obvious cause, people may feel dismissed or misunderstood. They may worry about serious illness. Clear explanation from healthcare providers can restore a sense of control.
Treatment of referred pain focuses on the true source. Addressing only the perceived location often provides little relief. If gallstones cause shoulder pain, removing the gallbladder resolves both issues. If cardiac ischemia triggers arm discomfort, restoring blood flow addresses the underlying danger.
Symptomatic relief may still play a role. Anti-inflammatory medications, physical therapy, or nerve blocks can reduce discomfort while the root cause is treated. But without identifying origin, relief may be temporary.
Recognizing emergency patterns is critical. Sudden left arm or jaw pain accompanied by chest pressure, sweating, or breathlessness warrants immediate medical evaluation. Severe upper back pain with abdominal symptoms may signal pancreatic or aortic pathology. The body sometimes whispers before it screams.
Awareness empowers decision-making. If pain persists without clear explanation, or if it does not respond to typical local treatment, consider the possibility of referral. Share full symptom details with a healthcare professional. Location alone does not define cause.
Referred pain reminds us that the nervous system prioritizes protection over precision. Evolutionarily, it was more important to generate an alert than to perfectly map the source. That protective bias explains why visceral pain often feels diffuse and why the brain may default to familiar surface areas when interpreting ambiguous signals.
This phenomenon is not a flaw but a byproduct of a complex, efficient system. The spinal cord acts as a hub. The brain acts as an interpreter. When multiple signals converge, interpretation can blur.
Medical science continues to study pain pathways, neural plasticity, and central processing. Research referenced in clinical overviews such as those published by Cleveland Clinic and educational summaries in Encyclopædia Britannica reinforces that referred pain is predictable and physiologically grounded, not psychological fabrication.
For patients, the most important takeaway is this: pain location does not always equal pain origin. If something feels off, especially when pain appears without clear injury, look deeper. Notice patterns. Observe triggers. Seek evaluation when symptoms are severe, persistent, or accompanied by systemic signs.
Understanding referred pain reduces fear and sharpens awareness. It bridges the gap between sensation and meaning. When you recognize that your nervous system sometimes reroutes signals, you gain clarity. And clarity transforms uncertainty into informed action.
Pain is communication. Referred pain is miscommunication—but purposeful miscommunication shaped by neural architecture. By learning its language, you become better equipped to interpret your body’s messages and respond wisely.
In the end, referred pain is a reminder that the body is interconnected in ways we rarely consider. Organs, muscles, skin, and brain share pathways woven together long before birth. When one area suffers, another may speak. Listening carefully, and understanding why the voice may sound displaced, is the key to responding correctly.
Sources:
Cleveland Clinic “Referred Pain: What It Is, Causes & Treatment”; Encyclopedia Britannica “Referred pain”; Healthline “What Is Referred Pain?”; peer-reviewed medical literature on convergence-projection theory and visceral pain mechanisms.