Electric-like pain is one of the most startling sensations the human body can produce. It does not creep in gradually like muscle soreness, nor does it throb steadily like an inflamed joint. Instead, it strikes — fast, sharp, and intense — often described as a lightning bolt, a sudden jolt, a zap that seems to come from nowhere. For many people, this type of pain is deeply unsettling because it feels abrupt, powerful, and unpredictable. The question that naturally follows is: why does it feel this way?
To understand why electric-like pain feels sudden and shocking, we must first understand how pain works in the body. Pain is not simply a reaction to injury; it is a complex communication system. The nervous system, composed of the brain, spinal cord, and peripheral nerves, constantly transmits electrical signals. These signals allow us to feel temperature, touch, pressure, and discomfort. In a healthy system, these signals are carefully regulated and interpreted accurately by the brain. However, when something disrupts this communication pathway, the signals can become distorted. That distortion is often what creates the sensation people describe as “electric.”
Electric-like pain is most commonly associated with neuropathic pain, a type of pain that arises from the nerves themselves rather than from damaged tissue. Unlike nociceptive pain, which occurs when specialized receptors detect injury or inflammation, neuropathic pain happens when the nerve fibers misfire, become irritated, or lose their protective insulation. In this case, the nerve is not just sending a warning about tissue damage — it is malfunctioning. When nerves misfire, they can discharge rapidly and unpredictably, producing sensations that feel like shocks, stabs, or jolts.
The reason this pain feels so sudden lies in the way nerve impulses travel. Nerve cells communicate through rapid electrical changes across their membranes. When functioning normally, these impulses are triggered by a stimulus — heat, pressure, or injury. But when a nerve is irritated or damaged, it may fire spontaneously. This spontaneous firing does not build gradually; it happens in milliseconds. The brain receives the message instantly, and because pain signals are designed to signal danger, the experience is intense and attention-grabbing.
Another reason electric-like pain feels shocking is the involvement of fast-conducting nerve fibers. Some nerve fibers are designed for speed, transmitting sharp, immediate pain signals so that we can quickly react to threats. When these fibers are involved in neuropathic conditions, the result is not a dull ache but a crisp, high-intensity sensation. It feels similar to touching a live wire — even though no electricity from outside the body is involved. The similarity comes from the nature of the nerve discharge itself.
Conditions affecting the peripheral nervous system often produce this type of pain. Peripheral neuropathy, which can occur due to diabetes, vitamin deficiencies, autoimmune conditions, or toxic exposures, frequently causes electric shock sensations in the hands and feet. When the protective myelin sheath around nerves is damaged, signals can leak or jump between fibers inappropriately. This abnormal cross-talk amplifies sensation and creates the perception of sudden zapping pain. People may notice that even light touch or minor movement triggers an intense electric feeling, because the nerve pathways have become hypersensitive.
Compression of nerves is another common cause. A herniated spinal disc pressing against a nerve root, or compression of the median nerve in carpal tunnel syndrome, can cause erratic nerve signaling. The mechanical pressure disrupts normal transmission, leading to bursts of activity that the brain interprets as shock-like pain. Often this pain travels along the path of the nerve, which is why someone with a compressed spinal nerve might feel electric pain radiating down an arm or leg.
Electric-like pain is also a hallmark feature of certain neuralgias. Trigeminal neuralgia, for example, is widely known for producing intense, lightning-like facial pain. In this condition, the trigeminal nerve becomes hyper-excitable, often due to compression or demyelination. Even mild triggers such as chewing, brushing teeth, or a light breeze can provoke explosive jolts of pain. The suddenness of the attacks reflects the nerve’s unstable firing pattern. The nerve does not gradually increase activity — it discharges abruptly, creating the shock sensation.
Central nervous system involvement can make the sensation even more complex. In conditions such as multiple sclerosis or central sensitization syndromes, the spinal cord and brain amplify incoming signals. When central pathways become overactive, even small peripheral inputs can feel dramatic. The nervous system essentially turns up the volume on pain perception. The resulting experience can feel like electrical surges running through the body, sometimes occurring without any clear external trigger at all.
The emotional impact of electric-like pain cannot be overlooked. Pain that is sudden and intense activates the body’s threat response. The brain is wired to treat sharp, rapid pain as urgent. This means adrenaline may rise, muscles may tense, and anxiety can follow. Over time, this cycle can heighten sensitivity further. When the brain anticipates pain, it may become more vigilant, amplifying future sensations. This is one reason why chronic neuropathic pain often feels unpredictable and distressing — it engages both the sensory and emotional circuits of the brain.
Interestingly, not all electric-like pain indicates structural damage. In some cases, the nervous system becomes functionally dysregulated. Fibromyalgia and other chronic pain syndromes demonstrate how altered pain processing alone can produce shock-like sensations. In these cases, imaging tests may not reveal visible nerve injury, yet the pain is real and biologically grounded. The nervous system has entered a state of heightened responsiveness, and the threshold for firing pain signals has dropped. Even subtle internal fluctuations can create intense sensations.
Medication withdrawal syndromes can also cause what people describe as “brain zaps” — brief electric shock sensations in the head. Though the exact mechanism is still being studied, it is believed that changes in neurotransmitter levels temporarily disrupt normal signaling patterns. This again underscores that electric-like pain is fundamentally about signaling instability rather than external electrical exposure.
The unpredictability of electric pain adds to its shocking quality. Unlike inflammatory pain, which often worsens gradually and correlates with movement or strain, neuropathic jolts can occur at rest. A person might be sitting quietly when a sudden zap travels down a limb. This unpredictability reinforces the sense of alarm. The brain struggles to identify a clear cause, which can increase anxiety and attentional focus on bodily sensations.
Diagnosis of electric-like pain requires careful evaluation because it is a symptom, not a standalone disease. Physicians may conduct neurological examinations, imaging studies, nerve conduction tests, and blood work to identify underlying contributors such as metabolic imbalances or structural compression. Understanding the source is essential because treatment varies depending on the mechanism involved.
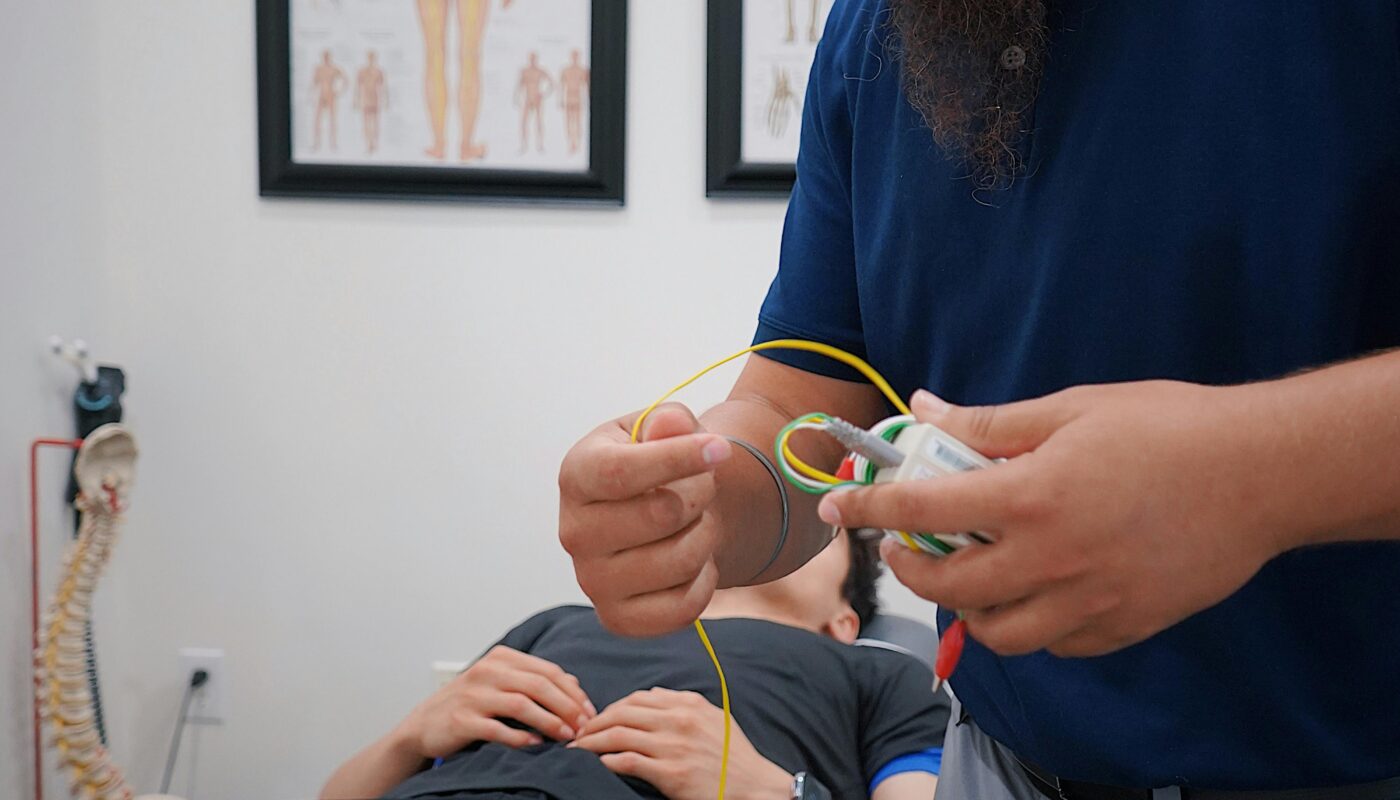
Treatment often differs from approaches used for typical inflammatory pain. Neuropathic pain medications target nerve signaling pathways rather than inflammation. Certain anticonvulsants and antidepressants can stabilize nerve firing and reduce abnormal discharges. Physical therapy may relieve compression-related causes. In some cases, interventional procedures or neuromodulation therapies are used to alter nerve signaling patterns directly.
Lifestyle factors also matter. Proper blood sugar control in diabetes can prevent progression of neuropathy. Adequate intake of essential nutrients such as vitamin B12 supports nerve health. Stress reduction techniques can calm central sensitization, decreasing overall nervous system excitability. Though electric-like pain feels dramatic, addressing underlying contributors often reduces both frequency and intensity over time.
It is important to recognize when electric-like pain requires urgent medical attention. Sudden shock sensations accompanied by muscle weakness, loss of coordination, changes in bladder or bowel control, or severe unexplained symptoms should be evaluated immediately. These may indicate significant nerve or spinal involvement. However, in many cases, electric pain, while distressing, is manageable once properly understood.
Ultimately, electric-like pain feels sudden and shocking because it originates in the body’s own electrical communication system. Nerves are designed to transmit rapid signals, and when those signals become unstable, the result is abrupt and intense. The shock sensation is not imaginary; it reflects real bioelectrical activity occurring within nerve fibers. The brain, interpreting that rapid discharge as danger, amplifies the experience.
Understanding this mechanism transforms fear into knowledge. What feels like an external electric force is actually an internal signaling disturbance. The nervous system, sensitive and complex, sometimes misfires. By identifying causes, stabilizing nerve activity, and supporting overall neurological health, it is possible to reduce both the shock and the uncertainty that accompanies it.
Electric-like pain may be startling, but it is not mysterious. It is a vivid reminder of how powerfully the nervous system shapes our experience of the world — and how even slight disruptions in its delicate circuitry can produce sensations that feel as dramatic as lightning itself.
Sources:
National Institute of Neurological Disorders and Stroke (NINDS) – Peripheral Neuropathy Fact Sheet; Cleveland Clinic – Neuropathic Pain Overview; Harvard Health Publishing – Understanding Nerve Pain; Mayo Clinic – Trigeminal Neuralgia; Johns Hopkins Medicine – Neuropathic Pain and Nerve Damage