Recurrent pain is one of the most frustrating and emotionally draining health experiences a person can face. It is not simply about discomfort returning. It is about the anticipation of pain, the disruption of plans, the erosion of confidence in one’s body, and the growing fear that relief will never be permanent. For many people, recurrent pain becomes a silent companion — unpredictable, intrusive, and deeply personal.
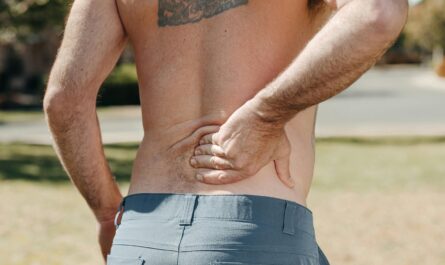
Whether it is migraines that strike every few weeks, lower back pain that resurfaces after physical activity, joint pain that flares seasonally, or abdominal pain that appears during stressful periods, recurring pain episodes rarely happen without pattern. They may feel random, but in most cases, they follow identifiable biological, behavioral, or environmental rhythms.
Understanding those patterns is the key to breaking the cycle. When people shift from asking “Why does this hurt again?” to “What keeps triggering this pattern?” they often begin to uncover powerful insights. Recurrent pain is rarely accidental. It is usually the result of layered contributors — nervous system sensitization, inflammation, posture, stress, sleep disruption, emotional memory, or lifestyle factors — interacting over time.
This article explores the most common patterns behind recurrent pain episodes, why they develop, and how recognizing them can open the door to meaningful, long-term change.
The Nervous System Pattern: When Pain Becomes Learned
One of the most significant drivers of recurrent pain is the nervous system itself. Pain is not just a signal from injured tissue; it is an experience created by the brain after interpreting signals from the body. When pain occurs repeatedly, the nervous system can become increasingly efficient at producing it.
This process, often referred to in medical literature as central sensitization, involves heightened responsiveness within the brain and spinal cord. Over time, the threshold for triggering pain lowers. What once required significant strain may eventually require very little. A minor movement, mild stress, or even anticipation can activate the pain response.
For example, someone who experienced a serious back injury years ago may find that even after tissues heal, episodes of back pain continue. The body is no longer damaged in the same way, but the nervous system has become primed to protect. The pain pathway has become well-rehearsed.
This pattern explains why imaging tests often fail to show new damage during flare-ups. The pain is real, but it is being driven by sensitivity rather than structural breakdown. The longer this cycle continues without retraining the nervous system, the more entrenched it becomes.
The Inflammation Pattern: A Fire That Never Fully Goes Out
Inflammation is essential for healing, but when it lingers at low levels, it can quietly contribute to recurring pain. Chronic low-grade inflammation does not always produce obvious symptoms until it reaches a tipping point. At that moment, pain flares.
This pattern is common in joint pain, autoimmune conditions, digestive disorders, and some types of headaches. Diets high in processed foods and sugar, chronic stress, poor sleep, obesity, environmental toxins, and underlying metabolic conditions can all maintain inflammatory activity in the body.
A person might notice that pain episodes follow periods of poor diet, illness, or emotional strain. The inflammation had been simmering beneath the surface, and a small trigger was enough to ignite a flare.
When recurrent pain is inflammation-driven, symptom relief alone rarely solves the issue. Anti-inflammatory medications may quiet the flare, but unless lifestyle contributors are addressed, the cycle often repeats.
The Biomechanical Pattern: Repetition Without Awareness
The human body thrives on movement variety, but modern life encourages repetition. Sitting at a desk for hours, driving long distances, looking down at a phone, or lifting objects incorrectly creates repetitive stress patterns.
Over time, these patterns cause muscle imbalances and strain connective tissue. Even if an acute episode resolves with rest or therapy, returning to the same movement habits often recreates the problem.
Recurrent neck pain, shoulder tension, and lower back discomfort frequently follow this pattern. A person may receive treatment, feel better, and assume the issue is resolved. However, if posture and movement mechanics remain unchanged, stress accumulates again until pain resurfaces.
The key to breaking this cycle is awareness. Subtle changes in workstation setup, strengthening weak muscle groups, and building regular movement breaks can dramatically reduce recurrence.
The Stress Pattern: Emotional Load as a Physical Trigger
Pain and stress are inseparable. Emotional strain activates the sympathetic nervous system — the body’s fight-or-flight response. Muscles tighten, breathing becomes shallow, stress hormones rise, and inflammation can increase.
For many individuals, pain episodes cluster during stressful periods. Tension headaches often emerge during deadlines. Gastrointestinal pain intensifies during conflict. Back pain resurfaces during emotionally heavy times.
The body does not distinguish sharply between physical and emotional threat. When stress becomes chronic, the nervous system remains on alert. Muscles never fully relax. Blood flow changes. Sleep quality declines. All of these factors make recurrent pain more likely.
Recognizing stress as a trigger does not mean pain is “all in your head.” It means the mind and body are deeply interconnected. Addressing stress through therapy, mindfulness, breathing techniques, or lifestyle adjustments can significantly reduce flare frequency.
The Sleep Disruption Pattern: When Rest Is Inadequate
Sleep is the body’s primary repair window. During deep sleep, tissues regenerate, inflammation decreases, and pain-modulating chemicals rebalance. When sleep is fragmented or insufficient, the body loses its ability to regulate pain effectively.
Research consistently shows that poor sleep increases pain sensitivity. People who experience insomnia are more likely to develop chronic pain conditions, and those with chronic pain are more likely to struggle with sleep. This bidirectional relationship forms a self-perpetuating loop.
Someone may notice that after several nights of inadequate sleep, pain becomes sharper or more widespread. Improving sleep hygiene often reduces both intensity and frequency of recurrent episodes.
The Fear-Avoidance Pattern: Protecting Too Much
After a painful episode, it is natural to avoid activities associated with discomfort. However, excessive avoidance can lead to deconditioning and heightened fear of movement.
Muscles weaken. Joints stiffen. Confidence declines. The nervous system begins to interpret movement as dangerous. Even harmless activities may trigger pain because they are perceived as threats.
This fear-avoidance cycle is common in back pain and post-injury recovery. The body is capable of healing, but protective behaviors persist long after healing should have occurred.
Gradual exposure to movement, guided rehabilitation, and reassurance help retrain both body and brain. Movement, when approached carefully and progressively, can reduce rather than increase pain sensitivity.
The Hormonal and Biological Rhythm Pattern
Some recurrent pain episodes follow biological cycles. Migraines, for example, may align with hormonal fluctuations. Autoimmune conditions may flare during times of immune stress. Women frequently report cyclical patterns of joint or pelvic pain associated with menstrual changes.
Recognizing cyclical patterns allows individuals to anticipate vulnerability windows and proactively adjust lifestyle factors such as stress, rest, and nutrition.
The Compensation Pattern: Pain Shifts Location
When one area of the body hurts, other areas compensate. A person with ankle pain may shift weight to the opposite leg. Over time, hip or back pain emerges. The original issue may improve, but secondary pain develops due to altered mechanics.
This shifting pattern can confuse patients who believe a new injury has occurred. In reality, the body has been redistributing stress.
Addressing compensation requires holistic assessment. Treating only the new pain location without understanding the underlying shift often leads to recurring issues in different regions.
The Environmental Pattern: Hidden Daily Triggers
Environmental factors are often underestimated. Unsupportive footwear, poorly designed workstations, heavy bags carried on one shoulder, or even mattress quality can contribute to recurring pain.
Because these exposures are constant, they gradually build strain. Pain flares may seem unpredictable, but when examined closely, they often follow prolonged environmental stress.
Making small environmental adjustments can dramatically alter pain patterns over time.
The Psychological Memory Pattern
Pain has memory. The brain stores experiences of injury and distress. When a situation resembles a past painful experience, the body may react defensively.
For example, someone who experienced severe back pain while lifting a heavy object may feel pain even lifting something lighter later. The brain anticipates danger and activates protective muscle tension.
Understanding that pain can be influenced by learned associations empowers individuals to work with professionals trained in cognitive behavioral therapy or pain reprocessing techniques to gradually diminish these conditioned responses.
Why Symptom-Only Treatment Fails
A recurring mistake in managing recurrent pain is focusing solely on symptom suppression. Medication may reduce inflammation or block pain signals temporarily, but if the underlying pattern remains unchanged, the episode returns.
True resolution requires asking deeper questions:
What circumstances surround each flare?
What changed before the pain intensified?
What physical, emotional, or behavioral patterns remain unaddressed?
Without examining these layers, treatment becomes reactive rather than preventive.
Breaking the Cycle of Recurrence
The path forward begins with observation. Keeping a detailed pain journal often reveals connections between sleep, stress, diet, posture, and flare-ups. Over weeks, patterns become visible.
Improving sleep hygiene, incorporating gentle strengthening exercises, managing stress proactively, adjusting ergonomics, and adopting anti-inflammatory dietary habits collectively create resilience.
Gradual nervous system retraining through consistent movement, exposure to previously feared activities, and psychological support reduces hypersensitivity. Healing is rarely instantaneous. It is cumulative.
Perhaps most importantly, individuals benefit from shifting perspective. Instead of viewing recurrent pain as a personal failure or mysterious curse, it can be reframed as a signal — a message that certain systems are under strain.
A Compassionate Perspective
Living with recurrent pain is exhausting. It challenges patience and confidence. It can make people doubt their own bodies. But patterns offer hope. If pain follows patterns, it can also be influenced by altering them.
Small, consistent changes often outperform dramatic but short-lived interventions. The body is adaptable. The nervous system can recalibrate. Inflammation can decrease. Muscles can strengthen. Fear can soften.
Recurrent pain episodes are rarely random. They are usually the visible surface of deeper rhythms — nervous system sensitivity, stress accumulation, inflammation, sleep disturbance, compensation, and learned protective responses.
When those rhythms are understood, the cycle can begin to shift.
Pain may return from time to time — but its frequency, intensity, and hold over life do not have to remain the same.
Sources:
Mayo Clinic – Chronic Pain Overview; National Institutes of Health – Pain and the Brain; Cleveland Clinic – Sleep and Chronic Pain; Journal of Pain Research – Central Sensitization Mechanisms; Harvard Health Publishing – The Role of Inflammation in Pain