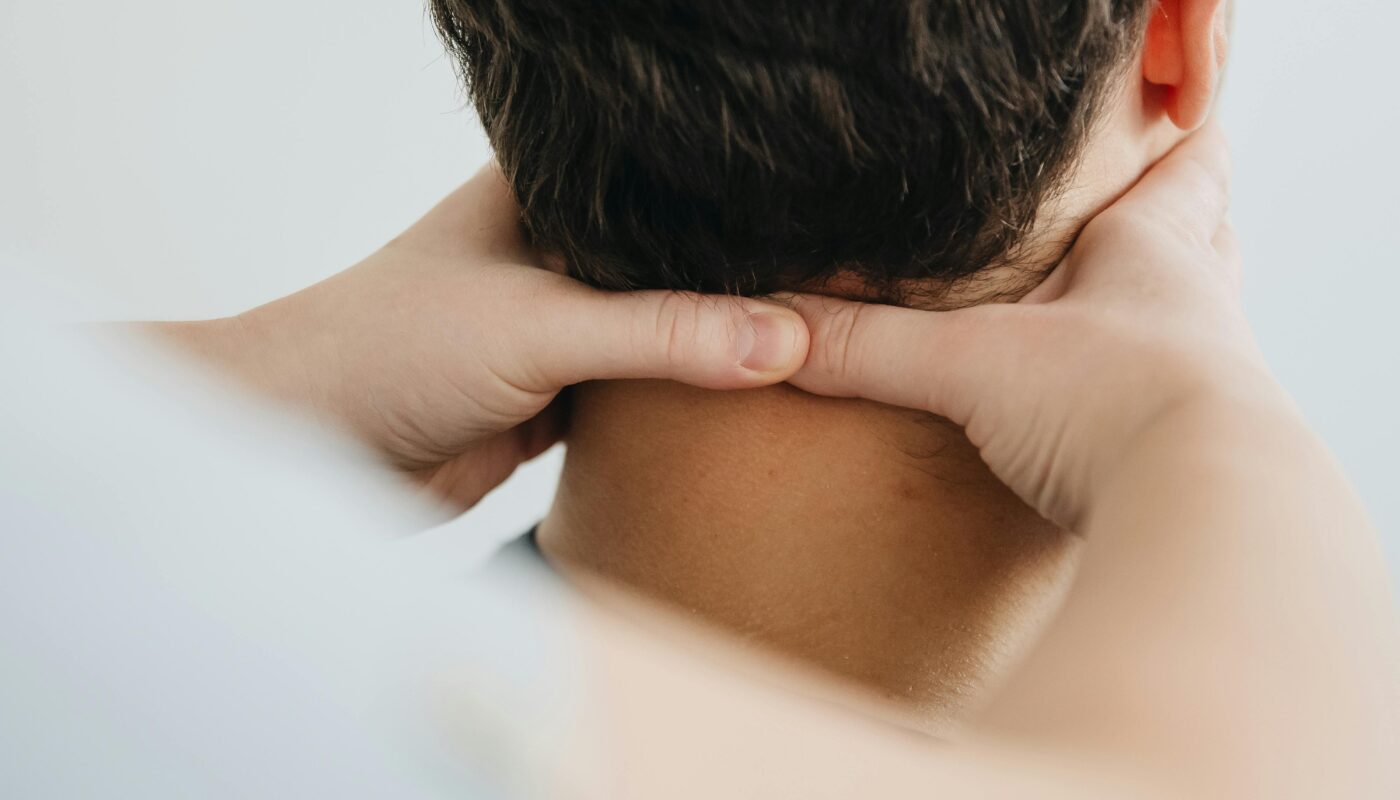
In today’s fast-paced world, stress is often described as something we “feel.” Yet, for millions of people, stress is not just an emotional experience—it is something they carry in their bodies. Tight shoulders, clenched jaws, aching backs, headaches, and unexplained fatigue are not random occurrences. They are the body’s language—physical expressions of emotional strain.
If you’ve ever wondered why anxiety makes your neck stiff, why deadlines trigger headaches, or why unresolved emotions seem to settle in your muscles, you are not alone. This article explores the deep, fascinating, and often misunderstood connection between emotional stress and physical tension—revealing the biological, neurological, and psychological pathways that transform invisible stress into tangible discomfort.
Understanding Stress: More Than a Feeling
Stress is not just a mental state—it is a full-body physiological response. When you encounter a stressful situation—whether it’s a looming deadline, relationship conflict, or financial worry—your body reacts as if it’s facing a real physical threat.
This reaction is known as the fight-or-flight response, a survival mechanism designed to protect you from danger. According to research, this response triggers a cascade of changes: increased heart rate, rapid breathing, and—crucially—muscle tension .
At its core, stress activates a system involving the brain and hormones:
- The amygdala detects danger
- The hypothalamus signals the body
- The pituitary gland and adrenal glands release stress hormones like cortisol
This system, known as the HPA axis, ensures your body is ready for action. But here’s the key problem: your body doesn’t distinguish well between physical danger and emotional stress.
So, whether you’re escaping a predator or worrying about an email, your body reacts in nearly the same way.
The Immediate Link: Why Stress Causes Muscle Tension
One of the fastest physical responses to stress is muscle contraction.
When stress hormones flood your body:
- Muscles tighten to prepare for action
- Blood is redirected to major muscle groups
- Your body becomes physically “on guard”
This is not accidental—it’s intentional. Tense muscles are better prepared for quick movement or defense.
According to health research, muscle tension is a standard part of the stress response, occurring alongside increased heart rate and blood pressure .
But What Happens When Stress Doesn’t End?
In short bursts, this tension is harmless—even helpful. But modern stress is rarely short-lived. Instead of minutes, it lasts for days, weeks, or even years.
And your muscles don’t know when to let go.
Chronic Stress: When the Body Gets Stuck in “On Mode”
The real issue begins when stress becomes chronic.
Instead of activating and resolving, the stress response stays partially “on,” like an engine idling too high for too long. This prolonged activation keeps muscles in a semi-contracted state.
Over time, this leads to:
- Persistent stiffness
- Reduced flexibility
- Pain and soreness
- Fatigue
Scientific evidence shows that chronic stress keeps the HPA axis activated, maintaining elevated cortisol levels and sustained physical tension .
This is why you may feel physically exhausted even if you haven’t done any strenuous activity—your muscles have been working overtime without rest.
The Role of Cortisol: The Silent Driver of Tension
Cortisol is often called the “stress hormone,” and for good reason. It plays a central role in how emotional stress becomes physical tension.
When stress is perceived:
- Cortisol mobilizes energy
- Increases blood sugar
- Alters immune function
- Keeps the body alert
But prolonged cortisol exposure has unintended effects.
Research highlights that chronic stress disrupts cortisol regulation, affecting multiple body systems and contributing to inflammation and physical discomfort .
How Cortisol Leads to Muscle Tightness
- Keeps muscles slightly contracted
- Reduces recovery and relaxation signals
- Promotes inflammation in tissues
- Heightens sensitivity to discomfort
In essence, cortisol turns temporary tension into long-term stiffness.
The Nervous System Connection: Why You Feel “Tight”
Your nervous system plays a crucial role in translating emotional stress into physical sensations.
There are two key branches:
1. Sympathetic Nervous System (Stress Mode)
- Activates fight-or-flight
- Increases muscle tension
- Heightens alertness
2. Parasympathetic Nervous System (Relaxation Mode)
- Promotes rest and recovery
- Releases muscle tension
- Slows the body down
Under chronic stress, the sympathetic system dominates. The parasympathetic system—the one responsible for relaxation—gets suppressed.
This imbalance keeps your body locked in a state of readiness, even when there is no real threat.
Emotional Suppression and Stored Tension
Not all stress is expressed outwardly. In fact, some of the most damaging stress is the kind we suppress.
When emotions like anger, fear, or sadness are not processed:
- The brain continues signaling “threat”
- The body maintains tension as a protective response
- Muscles become a storage site for unresolved stress
This is why people often report:
- Tight shoulders during responsibility overload
- Jaw clenching during anxiety
- Chest tightness during emotional distress
While the exact mapping of emotions to body parts is not strictly scientific, the general principle is valid: emotional states have physical expressions.
Fascia: The Hidden Tissue That Holds Stress
Beyond muscles lies an often-overlooked structure called fascia—a web-like connective tissue that surrounds muscles and organs.
Recent insights suggest that fascia:
- Responds to stress
- Stores tension patterns
- Becomes stiff when under chronic strain
As highlighted in recent health discussions, fascia can hold both physical and emotional tension, contributing to that “stuck” feeling in the body.
When stress persists, fascia loses elasticity, making movement feel restricted and uncomfortable.
Stress and Pain: A Two-Way Relationship
Stress doesn’t just cause tension—it also amplifies pain.
Research shows that stress and pain are deeply interconnected, sharing overlapping neural pathways .
How Stress Increases Pain Sensitivity
- Heightens nerve sensitivity
- Lowers pain threshold
- Reinforces “threat learning” in the brain
In chronic cases, stress can even lead to hyperalgesia, where the body perceives pain more intensely than usual.
This explains why minor aches feel worse during stressful periods.
The Feedback Loop: How Tension Creates More Stress
One of the most frustrating aspects of stress-related tension is that it becomes a self-reinforcing cycle.
- Emotional stress triggers muscle tension
- Tension causes discomfort or pain
- Pain increases emotional stress
- Stress further tightens muscles
Over time, this loop can lead to chronic pain conditions, even in the absence of physical injury.
Everyday Signs of Stress-Related Tension
Many people live with physical tension without realizing its emotional origin.
Common signs include:
- Tight neck and shoulders
- Jaw clenching or teeth grinding
- Frequent headaches
- Lower back stiffness
- Chest tightness
- Shallow breathing
- Fatigue without exertion
As shared in community discussions, individuals often notice that these symptoms appear during stressful periods and gradually fade when stress is reduced .
“The body holds stress physically, often without us noticing.”
Why Your Body Holds Stress Without You Noticing
One of the most surprising aspects of stress is how quietly it accumulates.
You may not feel “stressed” mentally, yet your body tells a different story.
This happens because:
- The brain processes threats subconsciously
- Micro-stressors accumulate throughout the day
- The body adapts to tension as a “new normal”
Over time, tension becomes so familiar that it feels invisible—until it turns into pain.
The Role of Posture and Modern Lifestyle
Modern habits amplify stress-related tension.
Key Contributors:
- Long hours sitting
- Poor posture (forward head, rounded shoulders)
- Screen overuse
- Lack of movement
These factors physically reinforce the stress response, making muscles more prone to tightening.
For example:
- Slouched posture compresses the chest
- Neck strain increases muscle load
- Reduced movement decreases circulation
Together, they create the perfect environment for tension to build.
The Science of Release: Why Stretching Feels So Good
Ever noticed how stretching during stress feels almost therapeutic?
That’s because:
- It interrupts the stress signal
- Restores muscle length
- Improves circulation
- Triggers dopamine release
Stretching also helps “reset” communication between the brain and muscles, reducing accumulated tension.
Breaking the Cycle: How to Release Emotional Tension
Understanding the connection between stress and tension is the first step. The next is learning how to interrupt the cycle.
1. Activate the Relaxation Response
Techniques like deep breathing and meditation can counteract stress by lowering cortisol and calming the nervous system .
2. Move Your Body
Gentle movement—walking, stretching, yoga—helps release stored tension and restore flexibility.
3. Become Body-Aware
Notice where you hold tension:
- Shoulders
- Jaw
- Back
Awareness is the first step toward release.
4. Address Emotional Triggers
Instead of ignoring stress, identify its source:
- Work pressure
- Relationship conflict
- Internal expectations
Processing emotions reduces the need for physical tension.
5. Improve Posture and Ergonomics
Small changes in how you sit, stand, and work can prevent tension buildup.
A Deeper Insight: Stress as a Whole-Body Experience
Perhaps the most important takeaway is this:
Stress is not just in your mind—it is in your entire body.
It influences:
- Hormones
- Muscles
- Nervous system
- Immune response
- Pain perception
This is why treating physical tension without addressing emotional stress often provides only temporary relief.
When to Seek Help
While stress-related tension is common, persistent or severe symptoms should not be ignored.
Seek professional guidance if you experience:
- Chronic pain
- Limited mobility
- Severe headaches
- Sleep disruption
- Anxiety or burnout
A combined approach—physical therapy, stress management, and psychological support—often yields the best results.
Final Thoughts
Emotional stress converting into physical tension is not a mystery—it is a deeply ingrained biological process. Your body is not malfunctioning; it is responding exactly as it was designed to.
But in a world where stress is constant and often invisible, this system can work against you.
The tight shoulders, aching back, and constant fatigue are not random inconveniences—they are signals. Signals that your body is carrying more than it should.
By understanding this connection, you gain the power to respond differently—to not just treat the symptoms, but to address the source.
Because sometimes, the most effective way to relax your body… is to listen to your mind.
Sources
Understanding the Stress Response – Harvard Health; Stress – NCCIH; The Role of Cortisol in Chronic Stress – PMC; Physiology, Stress Reaction – NCBI; The Interaction Between Stress and Chronic Pain – ScienceDirect