Pain is often expected to fade as the body heals. A cut closes, a surgery incision seals, and time is supposed to restore normalcy. But for many people, the story doesn’t end there. Instead, a new and often confusing chapter begins—one where pain persists, shifts, or even intensifies long after the visible wound has healed.
At the center of this experience lies a misunderstood biological process: scar tissue formation.
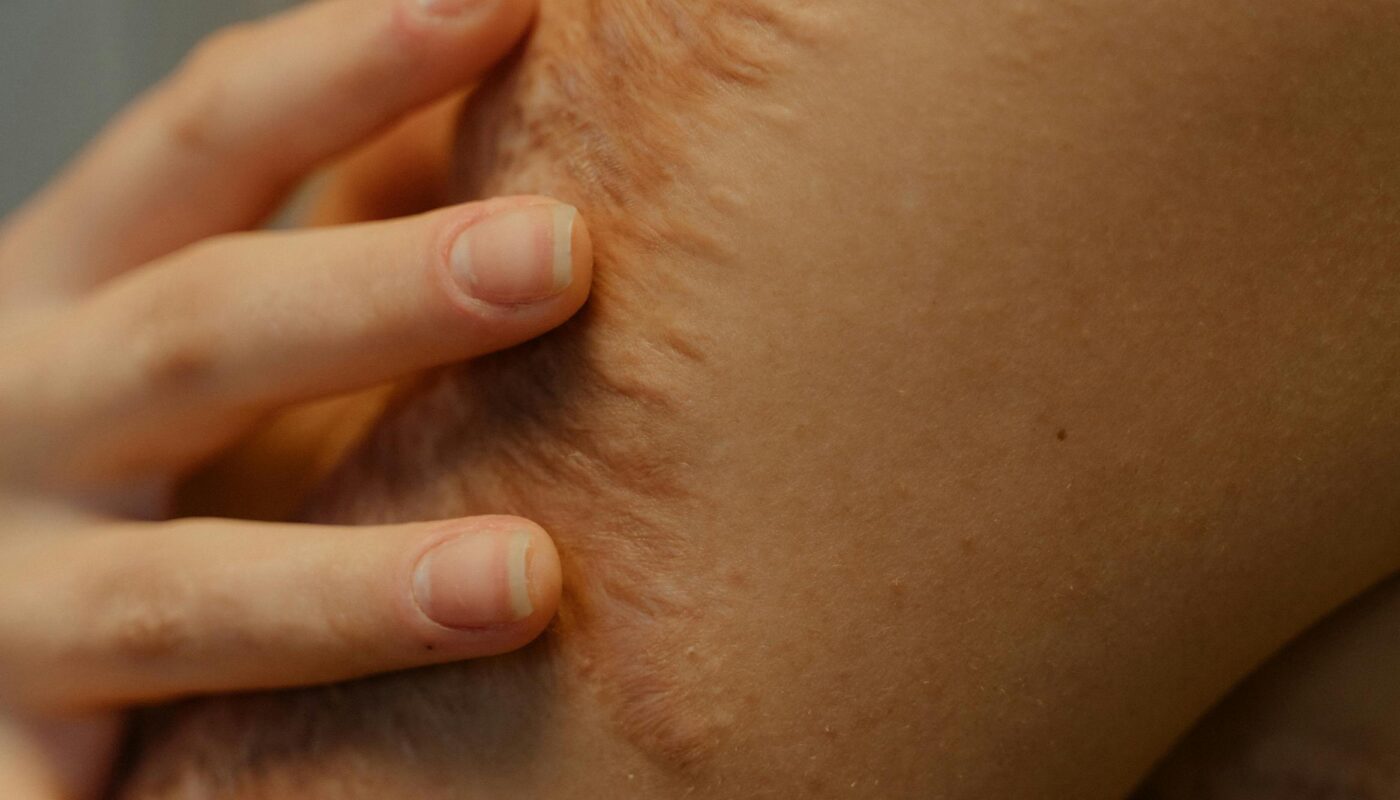
Scar tissue is not just a passive reminder of injury. It is active, dynamic, and deeply intertwined with how the body senses and processes pain. In some cases, it becomes a key driver of ongoing discomfort, stiffness, and even chronic pain conditions.
This article explores, in depth, how scar tissue forms, why it can become painful, and the mechanisms through which it influences ongoing pain sensations. More importantly, it connects these mechanisms to real-life pain experiences—helping readers understand what they are feeling and why.
Understanding Scar Tissue: More Than Just Healing
Scar tissue forms as part of the body’s natural healing response. When tissues are damaged—whether by injury, surgery, or inflammation—the body quickly works to repair the area using collagen fibers.
However, this repair process is not perfect.
Unlike healthy tissue, which has a flexible, organized structure, scar tissue is:
- Thicker
- Less elastic
- More densely packed
- Structurally different
In healthy skin or muscle, collagen fibers are arranged in multiple directions, allowing for flexibility and resilience. In scar tissue, these fibers align in a single direction, making the tissue stiffer and less adaptable.
This difference may seem subtle, but it has profound implications for how the body moves—and how it feels pain.
The Core Question: Why Does Scar Tissue Cause Pain?
Not all scars are painful. But when pain does occur, it is rarely due to a single cause. Instead, it emerges from a combination of mechanical, neurological, and inflammatory factors.
Let’s break these down.
1. Mechanical Tension: When Movement Becomes Restricted
One of the most immediate ways scar tissue contributes to pain is through restriction.
Because scar tissue is less elastic, it can:
- Pull on surrounding tissues
- Limit joint mobility
- Create abnormal tension patterns
This is especially noticeable in areas that require frequent movement, such as:
- Knees
- Shoulders
- Spine
- Abdomen
Over time, this restriction leads to compensatory movement patterns. The body begins to move differently to avoid discomfort, placing strain on other muscles and joints.
This creates a cycle:
Scar stiffness → altered movement → increased strain → more pain
Many people don’t realize that their pain isn’t just at the scar site—it’s the result of a chain reaction throughout the body.
2. Nerve Involvement: The Hidden Driver of Persistent Pain
Perhaps the most significant contributor to ongoing pain is the relationship between scar tissue and the nervous system.
Nerve Damage and Regrowth
During an injury, nerves can be:
- Damaged
- Severed
- Compressed
As healing occurs, nerves attempt to regenerate. But this process is not always orderly.
Scar tissue can:
- Trap regenerating nerve endings
- Alter their growth direction
- Increase sensitivity
As a result, the area may become hypersensitive, leading to sensations such as:
- Burning
- Tingling
- Electric shocks
- Sharp or stabbing pain
Interestingly, scar tissue may not be painful immediately. Pain can develop later as nerve endings regrow and interact with the scar environment.
3. Nerve Entrapment and Adhesions
In some cases, scar tissue forms adhesions—bands of fibrous tissue that bind structures together that are normally separate.
These adhesions can:
- Restrict nerve movement
- Compress nerves
- Create friction during movement
When a nerve is unable to glide freely, even simple movements can trigger pain signals.
This explains why some people experience pain only during specific motions, such as:
- Reaching overhead
- Bending
- Twisting
It also explains delayed pain—when discomfort appears months or even years after the initial injury.
4. Chronic Inflammation: A Lingering Signal
Inflammation is essential for healing. But when it doesn’t resolve properly, it becomes a source of ongoing pain.
Scar tissue formation involves:
- Activation of fibroblasts (cells that produce collagen)
- Release of inflammatory chemicals
- Remodeling of tissue over time
If this process becomes dysregulated, it can lead to fibrosis—an excessive buildup of scar tissue.
Fibrosis is associated with:
- Persistent inflammation
- Tissue thickening
- Reduced function
Fibroblasts that fail to deactivate can maintain a low-level inflammatory state, contributing to ongoing discomfort.
5. Biochemical Sensitization: Why the Area Feels “Overreactive”
Scar tissue is not just structurally different—it is chemically active.
During scar formation, the body releases substances such as:
- Cytokines (inflammatory signals)
- Growth factors
- Neurotransmitters
These chemicals can:
- Increase nerve sensitivity
- Lower the threshold for pain
- Amplify responses to touch or pressure
For example, molecules like Substance P and nerve growth factor play a role in both healing and pain signaling, linking scar formation directly to heightened pain perception.
6. Central Sensitization: When the Brain Joins the Loop
Pain is not just a local experience—it is processed by the brain.
When scar-related pain persists, the nervous system can become sensitized. This means:
- The brain becomes more responsive to pain signals
- Non-painful stimuli may feel painful
- Pain can persist even without ongoing tissue damage
This phenomenon, known as central sensitization, is a key factor in chronic pain conditions.
Scar tissue can act as a continuous source of input, keeping the nervous system in a heightened state of alert.
7. Delayed Pain: Why It Can Appear Years Later
One of the most frustrating aspects of scar-related pain is its unpredictability.
Many people report:
- Pain appearing long after healing
- Symptoms worsening over time
- New discomfort in previously stable scars
There are several reasons for this:
- Scar tissue matures slowly, sometimes over years
- Nerve regeneration changes sensation over time
- Mechanical stress accumulates
- Aging reduces tissue flexibility
Scars can take up to two years to fully mature, and their impact may continue evolving beyond that point.
8. Internal Scar Tissue: The Invisible Contributor
Not all scar tissue is visible.
Internal scarring can occur after:
- Surgeries
- Infections
- Chronic diseases
Examples include:
- Abdominal adhesions
- Lung fibrosis
- Liver cirrhosis
These internal scars can interfere with organ function and create deep, persistent pain.
For instance, scar tissue in joints or organs can lead to stiffness and discomfort, even without visible signs.
9. The Role of Movement and Load
Scar tissue is highly responsive to mechanical stress.
- Too little movement → stiffness increases
- Too much stress → irritation and inflammation
This creates a delicate balance.
When movement is limited, scar tissue becomes more rigid. When overloaded, it becomes irritated. Both scenarios can increase pain.
This is why gradual, guided movement is often essential in recovery.
10. Emotional and Psychological Impact
Pain is never purely physical.
Ongoing discomfort from scar tissue can lead to:
- Fear of movement
- Anxiety about reinjury
- Frustration and helplessness
These emotional responses can amplify pain perception, creating a feedback loop:
Pain → fear → reduced movement → more stiffness → more pain
Breaking this cycle requires both physical and psychological strategies.
Practical Implications: What This Means for People in Pain
Understanding the role of scar tissue changes how we approach pain.
It explains why:
- Pain doesn’t always match the visible injury
- Imaging may not fully explain symptoms
- Treatments focused only on inflammation may fall short
Instead, effective management often involves a combination of:
- Movement therapy
- Manual techniques
- Nervous system regulation
- Gradual exposure to activity
Key Takeaways
Scar tissue is not just a passive byproduct of healing—it is an active player in ongoing pain.
It influences pain through:
- Mechanical restriction
- Nerve involvement and entrapment
- Chronic inflammation
- Chemical sensitization
- Nervous system changes
These mechanisms often overlap, creating complex and persistent pain experiences.
A New Perspective on Healing
If you are experiencing ongoing pain near an old injury or surgical site, it does not mean your body has failed to heal.
It means your body has healed in a way that requires further adaptation.
Scar tissue is part of that story—not the end of it.
With the right understanding and approach, it is possible to:
- Improve mobility
- Reduce sensitivity
- Restore function
- Regain confidence in movement
Healing, in this sense, is not just about tissue repair—it is about restoring harmony between structure, movement, and the nervous system.
Sources
Healthline – “Scar Tissue Pain: Treatment, Symptoms, Starting Years Later, More”; Medical News Today – “What to Know About Scar Tissue Pain” (2025 update); Bijlard et al. – “A Systematic Review on the Prevalence, Etiology, and Pathophysiology of Intrinsic Pain in Dermal Scar Tissue” (Pain Physician, 2017); Zhao – “Burn Scar Pain: From Mechanisms to Treatments” (Frontiers in Physiology, 2025); Huang & Ogawa – “The Vascular Involvement in Soft Tissue Fibrosis” (IJMS, 2020)