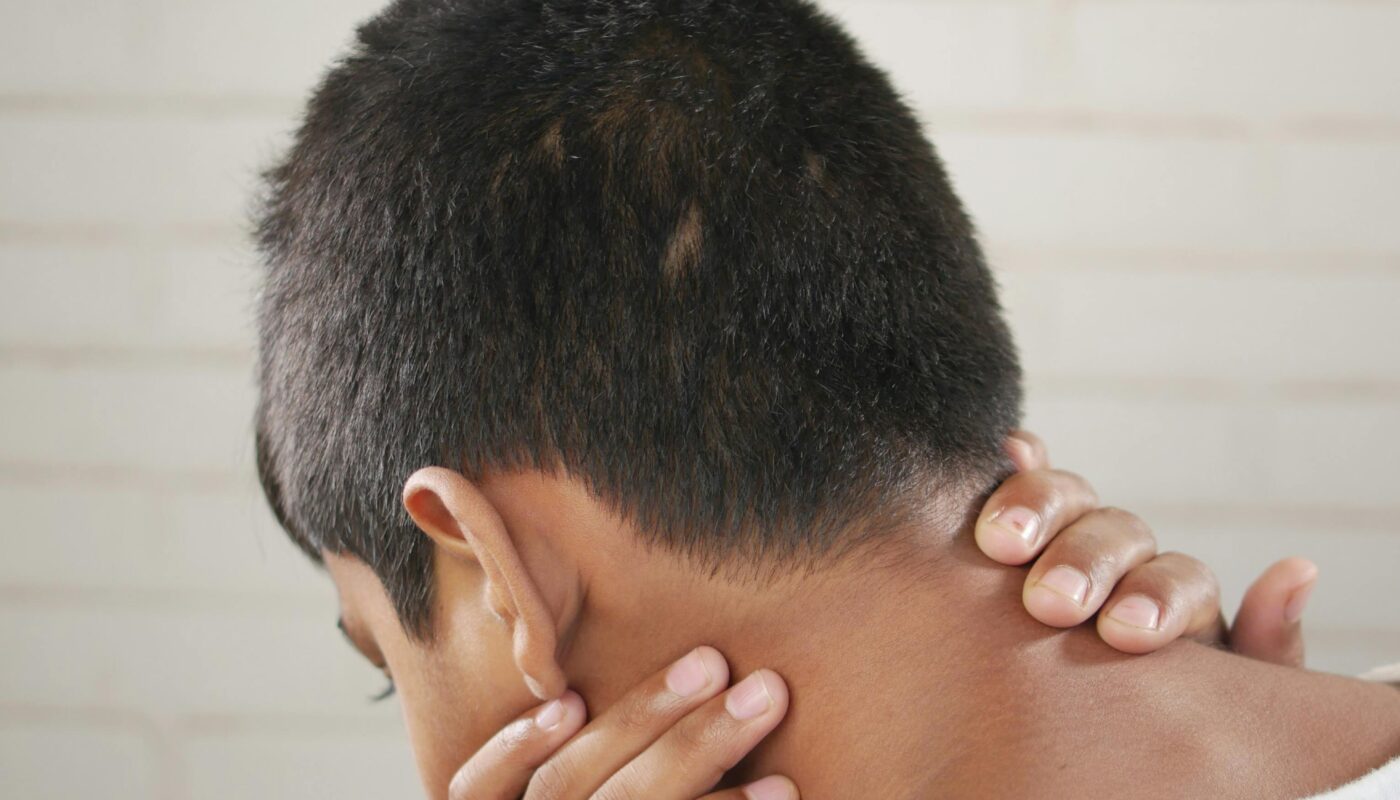
Pain is not a single, uniform experience. It can strike instantly like a sharp electric shock—or creep in hours later as a deep, spreading ache that seems harder to explain. This contrast often leaves people confused: Why does pain sometimes hit right away, and other times show up later—and why do they feel so different?
Understanding this difference isn’t just academic. It directly affects how people interpret injuries, manage recovery, and respond emotionally to discomfort. Immediate pain often feels urgent and precise, while delayed pain can feel vague, overwhelming, and even unsettling.
This article explores the biological, neurological, and psychological reasons behind this contrast—and why delayed pain often feels more complex, persistent, and harder to ignore.
The Two Timelines of Pain: Immediate vs Delayed
At its core, pain operates on two distinct timelines:
- Immediate pain (fast pain): Happens instantly after injury
- Delayed pain (slow pain): Develops minutes, hours, or even days later
These are not just timing differences—they are fundamentally different types of pain generated by different systems in the body.
Immediate Pain: The Fast Alarm System
Immediate pain is your body’s emergency alert.
When you touch something hot or twist your ankle, specialized nerve fibers called A-delta fibers rapidly transmit signals to your brain. These fibers are thinly myelinated (insulated), allowing them to conduct signals quickly—up to 30 meters per second.
This produces:
- Sharp, stabbing, or pricking sensations
- Highly localized pain (you know exactly where it is)
- Immediate awareness of danger
This type of pain is protective. It triggers reflexes—like pulling your hand away before serious damage occurs.
In simple terms:
Immediate pain is precise, fast, and survival-focused.
Delayed Pain: The Slow-Building Response
Delayed pain, on the other hand, comes from C-fibers—unmyelinated nerves that conduct signals much more slowly (0.5–2 m/s).
This leads to:
- Dull, aching, throbbing, or burning sensations
- Poor localization (hard to pinpoint exactly where it is)
- Gradual onset—minutes to days later
Unlike immediate pain, delayed pain is not just about detecting injury—it’s about processing damage and inflammation over time.
Delayed pain is diffuse, emotional, and persistent.
Why Delayed Pain Feels So Different
The differences in sensation are not random—they arise from several key biological and neurological mechanisms.
1. Different Nerve Fibers, Different Experiences
The most fundamental reason lies in how pain signals travel.
- Fast A-delta fibers → sharp, clear, immediate pain
- Slow C-fibers → dull, spreading, lingering pain
These fibers don’t just differ in speed—they also connect to different brain processing systems.
Fast signals go to areas responsible for location and intensity, while slow signals engage regions linked to emotion and discomfort.
That’s why delayed pain often feels:
- More exhausting
- More emotionally draining
- Less predictable
It’s not just slower—it’s processed differently by the brain.
2. Inflammation Takes Time to Build
Immediate pain happens at the moment of injury.
Delayed pain often emerges after the body begins repairing itself.
When tissue is damaged, the body releases chemicals like:
- Prostaglandins
- Histamine
- Cytokines
These create an “inflammatory soup” that sensitizes nerves and amplifies pain signals.
This process can take hours or days to peak.
Real-world example:
- You work out intensely → feel fine initially
- Next day → soreness and stiffness appear
This is not new damage—it’s your body’s repair process activating pain pathways.
3. Delayed Pain Is More Diffuse and Harder to Locate
Immediate pain is easy to pinpoint:
“My finger hurts right here.”
Delayed pain often feels like:
“My whole leg feels sore, but I can’t isolate it.”
Why?
Because C-fibers:
- Have broader receptive fields
- Activate multiple neurons
- Spread signals across wider areas
This leads to poor localization, making delayed pain feel more ambiguous and sometimes more threatening.
4. Central Sensitization Changes the Game
Delayed pain is often amplified by what happens in the spinal cord and brain, not just at the injury site.
After injury, the nervous system can become more sensitive—a process called sensitization.
This involves:
- Increased responsiveness of neurons
- Lower thresholds for pain signals
- Amplification of incoming signals
Over time, even mild stimuli can feel painful.
This explains why delayed pain can:
- Feel stronger than the original injury
- Last longer than expected
- Spread beyond the original area
These changes are part of neuroplasticity, where the nervous system adapts—but sometimes in ways that increase discomfort.
5. Delayed Pain Engages Emotional Processing More Strongly
Pain is not just physical—it’s emotional.
Delayed pain tends to involve:
- Limbic system (emotion processing)
- Memory-related brain regions
- Attention and perception networks
Because it unfolds slowly, your brain has more time to:
- Interpret the pain
- Attach meaning to it
- Focus on it
This can make delayed pain feel:
- More intrusive
- More stressful
- Harder to ignore
Immediate pain, by contrast, is often brief and action-oriented.
6. The Role of Attention and Context
Immediate pain demands attention—but only briefly.
Delayed pain lingers, which means your brain keeps revisiting it.
Research shows that pain perception depends on:
- Attention
- Expectation
- Emotional state
Delayed pain often appears when:
- You’re resting
- You’re less distracted
- Your brain has time to “notice” it
This makes it feel more intense—even if the physical damage hasn’t changed.
7. Adrenaline Masks Immediate Pain
During injury, the body often releases adrenaline, which can temporarily suppress pain.
This explains why:
- Athletes continue playing despite injury
- Pain sometimes appears only after the event
When adrenaline fades, the full experience of pain emerges—often as delayed discomfort.
8. Delayed Pain Reflects Ongoing Processes, Not Just Injury
Immediate pain = signal of damage
Delayed pain = signal of ongoing biological activity
Delayed pain often reflects:
- Tissue repair
- Immune response
- Muscle adaptation
- Nerve sensitization
That’s why it can feel:
- More persistent
- Less clearly tied to a single event
- More difficult to “fix quickly”
9. Why Delayed Pain Often Feels Worse
Many people report that delayed pain feels more intense or distressing than immediate pain.
This happens because it combines:
- Ongoing inflammation
- Nervous system sensitization
- Emotional processing
- Lack of clear cause
Unlike immediate pain, which has a clear trigger, delayed pain can feel uncertain and unpredictable—which increases distress.
10. The Psychological Impact of Delayed Pain
Delayed pain can affect how people think about their bodies.
Common reactions include:
- “Did I injure myself without noticing?”
- “Why is this getting worse instead of better?”
- “Is something seriously wrong?”
This uncertainty can increase:
- Anxiety
- Hypervigilance
- Pain perception itself
Pain is not just a signal—it’s an experience shaped by interpretation.
11. Everyday Examples of Delayed Pain
1. Post-exercise soreness (DOMS)
- Appears 24–48 hours later
- Caused by micro-damage and inflammation
2. Bruising
- Pain increases as swelling develops
3. Joint overuse
- Feels fine during activity
- Pain emerges later
4. Nerve irritation
- Delayed burning or tingling sensations
These examples highlight that delayed pain is often a process, not a moment.
12. Why Understanding This Matters
Recognizing the difference helps people:
- Avoid panic when pain appears later
- Understand recovery processes
- Respond appropriately to injury
For example:
- Immediate sharp pain → stop activity immediately
- Delayed soreness → may reflect normal adaptation
Misinterpreting delayed pain can lead to:
- Unnecessary fear
- Over-treatment
- Avoidance of healthy activity
13. When Delayed Pain Signals a Problem
While delayed pain is often normal, it can sometimes indicate:
- Significant inflammation
- Tissue damage
- Chronic pain conditions
Warning signs include:
- Pain worsening over time
- Pain lasting beyond expected healing
- Pain spreading significantly
- Associated symptoms (fever, numbness, weakness)
In such cases, medical evaluation is important.
14. The Bigger Picture: Pain Is a Process, Not a Moment
The key insight is this:
Pain is not just about what happened—it’s about what your body is doing afterward.
Immediate pain is a snapshot.
Delayed pain is a story unfolding.
Understanding this shift—from event to process—helps explain why delayed pain feels:
- More complex
- More emotional
- More persistent
Conclusion
Delayed pain feels different from immediate pain because it arises from entirely different biological systems and purposes.
- Immediate pain is fast, sharp, and protective
- Delayed pain is slow, diffuse, and tied to healing and adaptation
The involvement of slower nerve fibers, inflammatory processes, nervous system sensitization, and emotional brain networks all contribute to its unique character.
Rather than viewing delayed pain as confusing or alarming, it’s more accurate to see it as your body continuing the conversation long after the initial event has passed.
Understanding that difference can transform how you respond to pain—turning uncertainty into insight, and fear into informed awareness.
Sources
StatPearls – Physiology of Nociception; StatPearls – Pain Physiology; NCBI – Pathophysiology of Pain; AMBOSS – Nociception and Pain Modulation