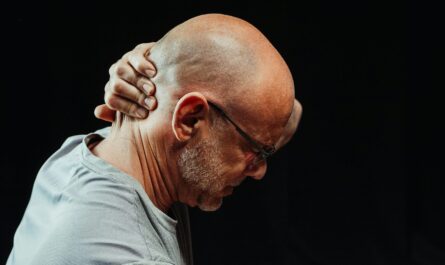
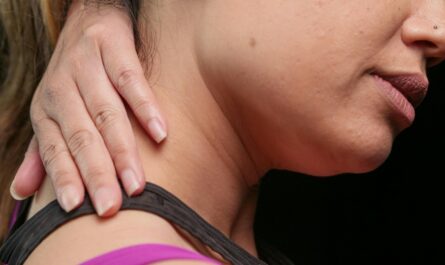
Pain rarely behaves the way we expect it to. When you twist your ankle, strain your back, or experience a stiff neck after a long day, you naturally assume the discomfort will remain confined to that exact spot. But for many people, that is not what happens. The pain lingers. Then it expands. What started as a small, localized ache gradually begins to involve surrounding tissues, neighboring joints, or even distant parts of the body. The experience can be confusing and alarming. People often wonder: Is something new wrong? Is the injury worsening? Why does pain seem to have a life of its own?
The truth is that pain spreading beyond its original area is a recognized and scientifically explained phenomenon. It does not necessarily mean new damage is occurring. Instead, it reflects the remarkable complexity of the nervous system, the adaptability of muscles and connective tissues, and the intricate relationship between physical injury, inflammation, movement patterns, and the brain’s interpretation of signals. Understanding why pain spreads is one of the most empowering steps a person can take when facing persistent discomfort.
Pain begins as a protective signal. Specialized nerve endings called nociceptors are embedded throughout the skin, muscles, joints, and internal organs. When these receptors detect potential harm—pressure, inflammation, chemical irritation, or tissue injury—they send electrical signals through peripheral nerves into the spinal cord and upward to the brain. The brain then interprets those signals as pain. This process is not mechanical or purely automatic. It is influenced by context, past experiences, emotional state, stress levels, and overall nervous system sensitivity. Pain is not just a sensation; it is an interpretation.
In acute injuries, this system functions efficiently. You strain a muscle, feel pain, protect the area, and heal. But when pain persists for days or weeks, the nervous system can begin to change. One of the most important reasons pain spreads is a process known as central sensitization. In this state, the spinal cord and brain become more responsive to pain signals. Neurons that once required strong stimulation to activate begin firing more easily. The threshold for discomfort lowers. Signals from nearby tissues that would normally be ignored start being amplified. As a result, pain can expand beyond its original boundaries.
Central sensitization does not mean the pain is imaginary. It means the nervous system has become hypersensitive. The brain essentially turns up the volume on incoming signals. This amplification can cause pain to feel more intense, more widespread, and longer-lasting than the original injury would suggest. Over time, areas adjacent to the injury begin to feel tender or sore, even if they were not initially harmed. The pain map in the brain enlarges.
Another explanation for spreading pain lies in the concept of referred pain. The body’s nerve pathways are not neatly separated. Sensory nerves from different regions often converge at the same spinal cord segments. When signals from one structure enter the spinal cord, the brain can misinterpret their origin. This is why a problem in one area can produce discomfort in another. A compressed nerve root in the lower back may generate pain that travels down the leg. A trigger point in the shoulder may produce aching in the neck or head. The spreading sensation feels real because the brain is interpreting overlapping nerve inputs.
Biomechanics also play a crucial role. When pain develops in one joint or muscle, the body instinctively adapts to avoid discomfort. You may shift your weight away from a painful knee, tilt your head to avoid neck tension, or change the way you lift objects to protect your back. These compensatory movements may reduce stress on the injured area temporarily, but they increase strain elsewhere. Muscles that were not designed to handle certain loads suddenly take on extra work. Over days or weeks, they become fatigued and irritated. What began as a localized issue transforms into a chain reaction affecting multiple regions.
Scar tissue formation and fascial restrictions can contribute as well. After injury or surgery, the body repairs damaged tissue by laying down collagen fibers. While this is essential for healing, scar tissue is often less elastic than the original tissue. It can bind adjacent structures together, limiting mobility. Reduced mobility alters movement patterns, and altered movement patterns create new stress points. Pain spreads not because the body is failing, but because it is adapting imperfectly to structural change.
Inflammation is another factor that can extend pain. When tissue is injured, the immune system releases chemical mediators such as cytokines and prostaglandins. These substances increase blood flow and sensitize nerve endings to promote healing. However, if inflammation becomes prolonged or excessive, surrounding tissues may also become sensitized. Neighboring nerves respond more intensely to stimulation, widening the area of discomfort. Chronic low-grade inflammation, common in conditions like arthritis, can slowly expand the region of pain over time.
Neuropathic mechanisms offer yet another explanation. When nerves themselves are damaged or compressed, they may begin firing spontaneously or erratically. This can create sensations that radiate along the length of the nerve. Tingling, burning, or electric-like pain often follows predictable pathways because nerves travel specific anatomical routes. In such cases, spreading pain reflects altered nerve signaling rather than spreading tissue damage.
Chronic pain conditions illustrate how powerful these mechanisms can become. In fibromyalgia, for example, individuals experience widespread pain without clear structural injury in every painful area. Research suggests that central sensitization plays a significant role, amplifying signals across the nervous system. What may have begun as localized pain evolves into a body-wide experience due to heightened neural responsiveness. Similarly, long-standing back pain may eventually involve the hips, upper back, or legs, not because multiple injuries occurred, but because the nervous system and movement patterns have adapted in ways that perpetuate discomfort.
Psychological and emotional factors also influence pain spread. Stress activates the sympathetic nervous system, increasing muscle tension and altering pain thresholds. When a person lives in a state of chronic stress, muscles remain partially contracted for extended periods. This tension reduces blood flow, promotes fatigue, and creates new areas of soreness. Anxiety about pain can heighten awareness of bodily sensations, amplifying the perception of discomfort. The brain, constantly scanning for threat, may interpret minor signals as significant. Over time, this heightened vigilance expands the perceived area of pain.
Sleep disruption further compounds the problem. Deep sleep stages are critical for tissue repair and nervous system regulation. Poor sleep increases inflammatory markers and lowers pain tolerance. When restorative sleep is absent, small aches can become more noticeable, and recovery slows. Pain becomes more persistent and more likely to spread.
Reduced activity is another contributor. When pain discourages movement, muscles weaken and joints stiffen. Immobility decreases circulation and limits the nourishment of tissues. As strength declines, everyday tasks place greater strain on the body. This cycle—pain leading to inactivity, inactivity leading to weakness, weakness leading to more pain—gradually enlarges the area of discomfort. The body becomes less resilient, and minor stresses produce exaggerated responses.
Neuroplasticity, the brain’s ability to change and adapt, plays a central role in this process. Every time pain is experienced, neural pathways involved in that sensation are reinforced. If pain persists, these pathways become stronger and more easily activated. It is similar to learning a skill: repetition builds efficiency. Unfortunately, in chronic pain, repetition builds sensitivity. The nervous system becomes adept at producing pain, even when the original injury has healed.
Despite how unsettling spreading pain can feel, it does not always signal worsening damage. In many cases, it reflects changes in how the nervous system processes information. This distinction is crucial. When people interpret spreading pain as evidence of new injury, fear increases. Fear can alter posture, reduce movement, and amplify stress hormones. This reaction reinforces the cycle of sensitization. Education about pain mechanisms often reduces fear and, in turn, reduces pain intensity.
However, not all spreading pain should be dismissed. Rapid progression of symptoms, especially when accompanied by weakness, numbness, fever, or systemic signs, requires medical evaluation. Infections, nerve compression, autoimmune conditions, and vascular problems can also present with spreading discomfort. The key difference lies in the pattern, severity, and associated symptoms.
Management of spreading pain involves addressing both the body and the nervous system. Gentle, graded movement is essential. Movement restores circulation, maintains flexibility, and signals to the brain that the body is safe to use. Gradual exposure to activity reduces fear and retrains the nervous system. Strengthening exercises help correct compensatory imbalances and distribute loads evenly across joints.
Pain neuroscience education has become an important component of modern rehabilitation. When individuals understand that pain can persist without ongoing damage, anxiety decreases. This cognitive shift reduces central amplification. Techniques such as mindfulness and controlled breathing calm the stress response, lowering muscle tension and sympathetic activation.
Sleep hygiene, anti-inflammatory lifestyle choices, and stress management further support recovery. In some cases, manual therapy or medications may be appropriate to reduce acute sensitivity and facilitate participation in rehabilitation. The goal is not simply to eliminate pain signals but to normalize how the nervous system interprets them.
Pain that spreads beyond its original area tells a story about adaptation. It reflects how interconnected the body truly is. Muscles influence joints. Nerves influence perception. Thoughts influence sensation. The body is not a collection of isolated parts but a dynamic network. When one part is stressed, others respond.
Understanding this interconnectedness transforms fear into insight. Instead of asking, “Why is my body falling apart?” a more accurate question becomes, “How has my nervous system adapted, and how can I guide it back toward balance?” In many cases, spreading pain is reversible. With appropriate movement, education, and support, the nervous system can recalibrate. Sensitivity can decrease. Areas that once felt chronically sore can quiet down.
Pain spreading does not mean weakness. It means the body and brain are responding—sometimes imperfectly—to stress, injury, and experience. By respecting the complexity of pain and addressing its biological, mechanical, and emotional dimensions, recovery becomes possible. The path forward often involves patience, consistency, and understanding, but it is a path grounded in science and hope.
Sources: Woolf CJ, “Central Sensitization: Implications for the Diagnosis and Treatment of Pain,” Pain; Treede RD et al., “Chronic Pain as a Disease,” Pain; Nijs J et al., “Central Sensitization in Chronic Pain Conditions,” Pain Physician; Clauw DJ, “Fibromyalgia: A Clinical Review,” JAMA; Butler DS & Moseley GL, Explain Pain