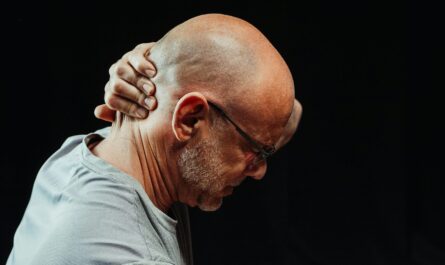
Pain is supposed to guide us. It’s meant to be a clear signal: “Something is wrong here.” But what happens when pain shows up somewhere completely different from where the problem actually is?
You feel discomfort in your shoulder—but the issue is your gallbladder. Your knee aches—but the real culprit is your hip. Your left arm hurts—but the danger lies in your heart.
This confusing phenomenon is called referred pain, and for many people, it is not just puzzling—it’s frustrating, anxiety-inducing, and sometimes even dangerous when it delays diagnosis.
In this in-depth article, we’ll explore why referred pain happens, how your nervous system “misroutes” signals, what science says about it, and why understanding it can dramatically improve your awareness of your own body.
What Is Referred Pain?
Referred pain is defined as pain that is felt in a location different from its actual source.
Unlike local pain, where the discomfort is felt exactly at the site of injury, referred pain creates a disconnect between cause and sensation.
For example:
- A heart problem may cause pain in the left arm
- A kidney issue may cause back pain
- A hip disorder may lead to knee pain
This is not random—it follows predictable neurological patterns.
The Core Problem: Your Brain Is Interpreting Signals Incorrectly
At the heart of referred pain lies a simple but powerful issue:
Your brain is making an educated guess—and sometimes it guesses wrong.
Pain signals travel from your body to your brain through complex nerve pathways. But these pathways are not always clean, separate highways. Instead, they often merge, overlap, and share routes.
This creates confusion.
The Convergence Theory: “Crossed Wires” in the Nervous System
The most widely accepted explanation for referred pain is called the convergence-projection theory.
What It Means
Multiple sensory nerves from different parts of the body can converge onto the same neurons in the spinal cord.
Think of it like several phone lines connecting to a single operator.
When a signal arrives, the brain must decide:
“Where did this come from?”
If two different body parts share the same pathway, the brain may misinterpret the source.
Real-Life Example
- Nerves from the heart and left arm enter the spinal cord at similar levels
- The brain is more familiar with signals from the arm than the heart
- So it interprets the pain as coming from the arm
This is why heart attacks often cause arm pain.
Why Internal Organs Are Especially Confusing
Referred pain is especially common with internal organs (viscera).
Low Pain Sensitivity
Internal organs:
- Have fewer pain receptors
- Send diffuse, poorly localized signals
This makes it harder for the brain to pinpoint the exact origin.
Shared Neural Pathways
Signals from internal organs often share pathways with skin and muscles.
So when your stomach sends a distress signal, your brain might interpret it as coming from:
- The abdomen
- The back
- Or even the chest
Dermatome Mapping: The Body’s “Pain Map”
Your body is organized into regions called dermatomes, each linked to specific spinal nerves.
When different tissues share the same spinal segment:
- The brain may project pain to the skin area (dermatome) instead of the deeper structure
For example:
- Heart → C5–T1 spinal segments → Left arm and chest pain
- Diaphragm irritation → Shoulder pain
This mapping explains why referred pain often follows predictable patterns.
The Role of the Brain: Pattern Recognition Over Precision
Your brain prioritizes speed and familiarity over accuracy.
Why?
From an evolutionary standpoint:
- Pain from skin or muscles is more common and immediate
- Internal organ pain is rarer and less well-mapped
So the brain uses a shortcut:
“This signal looks like something I’ve seen before—must be coming from there.”
This shortcut works most of the time—but fails in referred pain scenarios.
Central Sensitization: When the System Amplifies Confusion
In chronic pain conditions, the nervous system becomes more sensitive.
This is called central sensitization.
What Happens?
- Neurons in the spinal cord become hyperactive
- They respond more strongly to signals
- Pain spreads to wider areas
As a result:
- Referred pain becomes more intense
- The affected area becomes larger and harder to define
Why Referred Pain Feels So Real (and Misleading)
One of the most frustrating aspects of referred pain is that it feels completely genuine in the wrong location.
That’s because:
- The brain does not “label” pain as referred or local
- It simply produces the sensation where it believes the problem is
So if your brain thinks the issue is in your shoulder, your shoulder will hurt—even if it’s perfectly healthy.
Common Examples of Referred Pain
1. Heart → Arm, Neck, Jaw
A classic and potentially life-threatening example.
2. Gallbladder → Right Shoulder Blade
Often mistaken for muscle pain.
3. Kidney → Lower Back or Groin
Can mimic musculoskeletal issues.
4. Hip → Knee
Frequently misdiagnosed in orthopedic cases.
5. Trigger Points → Distant Muscle Areas
Muscle knots can send pain far from their origin.
Referred Pain vs Radiating Pain
These two are often confused, but they are very different.
Referred Pain
- Felt in a different location
- No direct path of pain
- Example: Heart → arm
Radiating Pain
- Travels along a continuous nerve pathway
- Example: Sciatica from back → leg
Understanding this distinction is crucial for diagnosis.
Why Diagnosis Becomes Difficult
Referred pain can mislead both patients and doctors.
Common Challenges
- Treating the wrong area
- Missing serious conditions (like heart disease)
- Confusing symptoms with unrelated issues
In some cases, patients feel dismissed because:
- The painful area appears normal
- Tests show no issue at the site of pain
This can lead to frustration and delayed treatment.
Emotional and Psychological Impact
Referred pain is not just physical—it affects mental well-being.
Common Experiences
- Confusion: “Why does my knee hurt if my knee is fine?”
- Anxiety: “Is something serious being missed?”
- Frustration: “Why can’t doctors find the cause?”
This uncertainty can amplify the perception of pain itself.
The Science Is Still Evolving
Despite decades of research, referred pain is not fully understood.
Several theories exist:
- Convergence-projection theory (most accepted)
- Axon reflex theory
- Cortical reorganization theory
- Convergence-facilitation theory
Each explains part of the puzzle—but no single theory explains everything.
Why the Body “Designed” This System
It may seem like a flaw, but referred pain likely has evolutionary roots.
Possible Reasons
- Efficiency
- Shared neural pathways reduce complexity
- Energy Conservation
- Fewer dedicated pathways for each organ
- Survival Priority
- Surface injuries (skin, muscles) needed faster, clearer signals
Internal organs, being less exposed, did not require precise localization.
How to Identify Referred Pain
While only a medical professional can diagnose it, some clues include:
- Pain location doesn’t match known injury
- Pressing the painful area doesn’t worsen pain
- Pain appears alongside symptoms elsewhere
- Pain patterns match known referral maps
When to Take It Seriously
Referred pain can sometimes signal serious conditions.
Seek immediate medical attention if you experience:
- Chest pain with arm/jaw discomfort
- Sudden unexplained back pain with other symptoms
- Persistent pain with no clear cause
Managing Referred Pain
Treatment focuses on the true source, not the painful area.
Approaches Include
- Physical therapy
- Addressing underlying organ issues
- Trigger point therapy
- Neurological pain management
Treating only the site of pain often provides little relief.
The Bigger Picture: Pain Is an Interpretation, Not Just a Signal
Referred pain reminds us of something profound:
Pain is not just a physical sensation—it is a brain-generated experience.
Your body sends signals, but your brain decides:
- Where the pain is
- How intense it feels
- What it means
And sometimes, that interpretation is imperfect.
Final Thoughts
Referred pain is one of the most fascinating—and frustrating—features of the human body. It challenges our assumptions about pain, forcing us to look deeper than the obvious.
Understanding it can:
- Prevent misdiagnosis
- Reduce anxiety
- Improve communication with healthcare providers
Most importantly, it teaches us that pain is not always where it seems—and that listening carefully to the body often means looking beyond the surface.
Sources
Britannica – Referred Pain; PMC – Referred pain: characteristics, possible mechanisms, and clinical management; Physiopedia – Referred Pain; Physiopedia – Neuro-Physiological Theories of Referred Pain; Physiotutors – Somatic & Visceral Referred Pain Explained; EBSCO – Referred Pain (Reflective Pain); NCBI – The Anatomy and Physiology of Pain